Without Dr. William Morgan the 2004 Red Sox World Series win would not exist–a true Boston Hero.
View original post 25 more words

Without Dr. William Morgan the 2004 Red Sox World Series win would not exist–a true Boston Hero.
View original post 25 more words
A 2010 study, Corporate Psychopathy: Talking the Walk, found that 3 to 6 percent of corporate employees may be responsible for the majority of ethical breaches in corporations, with corporate psychopathy tending to be concentrated at the higher levels of organizations.
This group here, Like-minded Docs, is largely responsible for what happens to any doctor referred to a state PHP because all of the medical directors of the “PHP-approved” assessment and treatment centers can be found right here.
So too can Bob Dupont and Greg Skipper who have introduced the non-FDA approved drug and alcohol LDTs. Stuart Gitlow, President of ASAM is also on the list.
This group is essentially in control of doctors and determines their fates and the percentage of psychopathy here is much much more than the 3-6% found at Enron.
Some of these doctors have done horrible things that most doctors would never do under any…
View original post 962 more words
Source: Letters From Those Abused and Afraid
I get many e-mails, letters and phone calls from doctors, nurses and others who have been abused by “professional health programs” (PHPs).
Most are anonymous. Afraid of being identified and punished by the PHP, very few leave comments on my blog revealing their names or potentially identifiable information.
This is understandable. By simply reporting “noncompliance” to the medical boards a state PHP can end their careers. As it was with the Inquisition this system relies above all else on silence and secrecy. Speaking out can result in “swift and certain consequences.”
They are afraid. Some are undoubtedly suffering from PTSD. Most have developed a “learned-helplessness” Many have reported abuse and even crimes to their medical societies, medical boards, law enforcement, the media and others only to have the door slammed in their faces.-myself included.. They have no advocacy or support and feel no one cares. Their locus of control, identify and self-worth have been suddenly ripped from them without recourse. There is no lifeline. Attempts at justice are often undermined by a concerted defiance of the truth by their medical boards and even the attorneys who are purportedly working for them but will not “bite the hand that feeds.”
PHPs are ostensibly Employee Assistance Programs (EAPs) for doctors in both mechanics and mentality. EAPs assist employees with substance abuse, personal problems and other issues. They do not diagnose or treat “patients” but refer to outside professionals who do. The critical difference between EAPs and PHPs is PHPs have mandated all assessment and treatment be done by their own. These “PHP-approved” facilities are economically and ideologically intertwined with the PHP. The conflicts of interest are serious and many.
PHPs also use non-FDA approved junk-science drug and alcohol testing they introduced. The procedural safeguards most EAPs use to protect the donor ( certified labs, FDA-approved validated tests, split-specimen, strict chain-of-custody, MRO review) have been reviewed. Unvalidated “personality” assessments they also introduces are being used in “disruptive” physician evaluations guaranteed to find “character defects” to justify monitoring contracts. They implement polygraphs despite the AMAs previous conclusion they are scientifically unsupportable.
It is an institutionally unjust system of coercion, control and abuse that is unregulated, opaque and protected. There is no answerability and they are accountable to no one.
But regulatory agencies have readily adopted policies not only unsupported by science and evidence-based research but outside the normative principles and practice of medicine.
Granting PHPs authority to limit assessments and treatment to their own facilities offends the fundamental rights of the individual.
Informed consent (or refusal) constitutes a basic rule of the lawfulness of medical practice according to national and state medical practice acts governing the profession. It is a basic principle of all published principles of medical ethics.
Involuntary treatment is motivated by either potential harm to others (for the good of society) or by need for treatment and/or potential self harm.
Involuntary treatment should be a confined to those gravely disabled by psychiatric disorders or substance abuse. It necessitates reflection under the ethical principles of autonomy and beneficence.
A single DUI, transient psychological issue such as grief or anxiety, and even sham peer-review can easily land a doctor into forced assessment and involuntary treatment at a “PHP-approved” facility.
Involuntary assessment and treatment involves legal, clinical ethical, and deontological consideration in its demarcation.
The economic and ideological aspects need to be considered here.
How is it this paradoxical assessment and treatment paradigm legitimized and justified within a profession that emphasizes evidenced based decision making and beneficence and autonomy as two of the basic principles of medical ethics?
To sell the “PHP Blueprint” to other EAPs it is necessary to prevent doctors from speaking the truth. Very few want their names, states or other unique identifiers published for fear of consequences and retaliation.
The letters here have only been posted after being approved by their authors. The letter below is a representative sample I received today. The concept of our colleagues having to undergo “back alley” surgery under this regime is incomprehensible to me. -MLL
I was a victim of human rights violations committed by the PHP farmed out the group called Maximus. While in the “Diversion program” with 18 month clean sober, over 130,000 invested to date, I fractured and dislocated my shoulder. When arriving in the ED I told the MD of my circumstances and requested a drug test as part of my in addition to standard radiographs. The ED MD ordered IV pain medication right away seeing my pain. I refused, until I could reach my “diversion nurse counselor”. The ED doc consulted Pain Management and Ortho given the added level of complexity. Ortho advised that they immediately give me dilaudid and place my fractured shoulder back in socket as my hand was numb and my pulses were weak., then I be admitted for surgery. When I finally reached the PHP monitor, her she told me that if I “take anything other than tylenol ( including for surgery)she would have my license” My team of 4 physicians now at this point( a hospitalist, ortho, PM and ED) all agreed that this was ill advised and I must have my shoulder placed back into socket immediately. That assuredly, this nurse knew not what she spoke and as soon as Monday morning came and they could contact the medical board….I would certainly be vindicated”post-procedure”, as even my contract read,that “medical care recommended by a reasonable licensed physician could not be prohibited” by participation in the program. I let the orthopedist, give me dilaudid and reduce my shoulder. I was admitted to the hospital for one week, while the Orthopod tried to induce me to have the surgery. Pain Management managed my acute pain, with full knowledge of my situation. All the doctors tried to contact the medical board to tell them of my unique surgery. That I should not be kicked out of the program. And, I should have the surgery I needed. The medical board took my license. Upon discharge from the hospital, the the medical board detectives came to my door to inform me, that I couldn’t work. I knew I could not even get myself dressed. When the board detectives came to take my license I had my hospital wrist band on one hand, and a wrist band circulating around our beach community of Ladera Ranch, for the little girl whom I was just featured in the newspaper and on TV for saving her life. They told me I was a danger to the public. My life fell apart. It has never been the same. I had already paid some 130-160,000 in fees to the PHP, and related expenses, even though I “had a strong case to fight the board” as one attorney said. I had no more money left. They had taken everything from me. My life was over. Suicide is something I still think about as I try to piece my life together. There were human rights violations occurring. There were anesthesiologist in Diversion forced to have “back alley” surgeries while in the program, at their friends surgery centers, using diprovan, as it wasn’t checked for. If you had a minor surgery or God forbid a situation such as mine….you were kicked out and lost everything.
Doctors are coming forward all over the country to tell their stories of abuse by Physician Health Programs, quasi-governmental agencies that were originally intended to provide help to physicians who were suffering from mental illness or substance abuse problems. Unfortunately, these agencies have grown into abusive vehicles run without oversight and with a complete disregard for due process.
These programs were originally intended to provide an avenue for physicians in need of help with mental health problems or substance abuse/addiction.
Although the programs were often initiated with the best of intentions, they are now riddled with corruption and often used by unscrupulous former addicts or felons who identify themselves as “specialists” in addiction medicine. Control of these programs was ceded to private entities formed as nonprofits. In fact, addiction medicine is only a “self-identified medical specialty.” ABMS certification became a pathway for disgraced doctors to find a new career in…
View original post 99 more words
State Physician Health Programs -coercion, control and abuse.
This anecdote concerning a gay doctor’s revelation he liked his non monogamous lifestyle leading to a forced acceptance of a “sex addiction” diagnosis, mandatory inpatient treatment and indoctrination into 12-step recovery was just posted on the physician social network SERMO. If the pattern looks familiar it is.
Physician Health Programs (PHPs) are non-profit NGOs that exist in every state ostensibly to help impaired doctors and protect the public from harm. PHPs have no regulation or oversight and have essentially removed all accountability. Under the ruse of protecting a doctors anonymity and providing confidentiality they have built barriers of opacity. Most doctors are unaware how they work unless they become involved with them and they are not on the radar of the public at large–they need to be.
Organized under the Federation of State Physician Health Programs, (FSPHP), state medical boards have abdicated their responsibility and consider them expert authority on all things related to physician health–a logical fallacy that has placed illegitimate and irrational authority in professional control of medicine once again proving that knowledge isn’t power and ignorance often reigns.
PHPs encourage confidential referrals for “warning signs” such as those on the list below from the Massachusetts PHP, PHS, Inc. and guarantee the reporters anonymity. All semblance of due process has been removed. Medical boards have given state PHPS complete and absolute managerial control over assessment, treatment and monitoring. PHPs are not healthcare providers but monitoring agencies. If a PHP recommends an “assessment” of a reported doctor there is no choice in the matter. No allowances for a second opinion, outside support or appeal exist.
This doctor was apparently reported to his state PHP because a patient thought she smelled alcohol on his breath. As it turned out, the accusation was bogus but by being honest and forthcoming about his sexual orientation in the interview the PHP mandated an “assessment.” for unrelated issues. A not uncommon scenario as reports of behavioral issues often end up with hair tests for alcohol and other substances resulting in mandated assessments for “substance use disorder” followed by a five-year monitoring contract with the PHP and weekly urine tests.
The PHP provides a list of three or four facilities drawn from the same pool of “PHP-approved” assessment and treatment centers. However, an audit of the N.C. PHP found no written objective criteria or quantitative measurements existed on how these assessment and treatment centers are “approved” by the PHP. The common denominator seems to be that these facilities are (1) 12-step ASAM directed, and (2) willing to “tailor” an assessment to support a predetermined diagnosis. It is, in fact, a rigged game. Unfortunately the medical boards have been duped into mandating assessments at these centers under threat of loss of medical license and specifically exclude non “PHP-approved” assessments.
This scaffold is also the unspoken and hushed major contributor to physician suicide—It is the elephant in the room no one speaks of out of fear of being targeted. Doctors who really need help for mental health, substance abuse or other issues are afraid to get it for fear of being reported to the PHP. Those already monitored are subject to all sorts of psychological, financial and emotional abuse.
The Federation of State Physician Health Programs (FSPHP) has a relationship with Pine Grove. It is one of the “PHP-approved” facilities and two of their staff, Phillip Hemphill, PhD and James C. “Jes” Montgomery, MD are are listed as Program Faculty at the FSPHP annual educational conference and business meeting on April 24-27, 2015 in Fort Worth Texas.
Political Abuse of Psychiatry
Political abuse of psychiatry is the “misuse of psychiatric diagnosis, detention and treatment for the purposes of obstructing the fundamental human rights of certain groups and individuals in a society. The coercive use of psychiatry represents a violation of basic human rights in all Cultures.
What has occurred in the medical profession is no different from China or the Soviet Union under totalitarian rule where dissent is disapproved, often punished, and those perceived as threats to the existing system can be effectively “neutralized with trumped up psychiatric illness” and by this stigmatization reputations were ruined, power was diminished, and voices were hushed.
Political abuse of psychiatry involves the deliberate action of diagnosing someone with a mental condition they do not have as a means of repression or control and if you do not believe it is occurring right here today then take a look here and here to see how they are colluding with commercial drug testing companies to engage in forensic fraud and the assessment and the treatment centers to fabricate data to support non-existent diagnoses.
“Sex Addiction” used as a tool to Discriminate
There has been a lot of “chatter” in PHP circles concerning “sex addiction” and I knew they had been aligning themselves and setting up specialized programs at certain facilities. It seemed unusual as many of the key players who erected and run this scaffold have themselves been involved in sexual misconduct. 
One of the architects of the current system, Dr. Robert Walzer, M.D., J.D. who was instrumental in tinkering with administrative and medical practice laws to remove the due process and appeal rights of doctors surrendered his license in 2001 due to inappropriate sexual relationships with patients. He was the co-author of the current physician health program paradigm.
Dr. Margaret bean-Byog, M.D, Chairman of the credentialing  committee for the first certification exam and ASAM president surrendered her medical license after being accused of sexually abusing one of her patients, a Harvard medical student who subsequently died by suicide.
committee for the first certification exam and ASAM president surrendered her medical license after being accused of sexually abusing one of her patients, a Harvard medical student who subsequently died by suicide.
 And the FSPHP seems to treat doctors involved in sexually related misconduct in a favorable light. Take for instance, Dr. James Peak, M.D., a child psychiatrist who was sent to prison on a federal child pornography conviction taken under the wing of the Montana PHP. After “proving” he only ‘”looked” at pornography of young boys but never abused any using a polygraph “lie-detector” test his license was reinstated in no time at all. His treatment includes going to one AA meeting and one 12-step sex addict meeting per week. My guess is they need more staff at the PHP or one of the assessment centers.
And the FSPHP seems to treat doctors involved in sexually related misconduct in a favorable light. Take for instance, Dr. James Peak, M.D., a child psychiatrist who was sent to prison on a federal child pornography conviction taken under the wing of the Montana PHP. After “proving” he only ‘”looked” at pornography of young boys but never abused any using a polygraph “lie-detector” test his license was reinstated in no time at all. His treatment includes going to one AA meeting and one 12-step sex addict meeting per week. My guess is they need more staff at the PHP or one of the assessment centers.
I had been wondering what the motivation was behind this focus on “sex addiction” and my suspicions seem to be correct.
I have since heard of a second case of a gay doctor being forced into his state Physician Health Program (PHP) in Alabama.
Once under the control of the PHP most doctors are afraid to come forward because of the “swift and certain” consequences imposed on them. All they have to do is say the doctor was “noncompliant” to the medical board and it is over. They lose their license and there is not a thing they can do about. it. I have heard from doctors in multiple states going to law enforcement, the Attorney General, the media and the ACLU only to have the door slammed in their faces. Myself included. .
The coercion, control, ethics, and civil and human rights violations remain hidden. The crimes remain hidden. So too will this.
It appears the FSPHP is following the same pattern they have with the “impaired” and “disruptive” physicians–to discriminate. The targeting of gay, lesbian or transgender doctors for what they do in their private lives is predictable. It is an inevitable part of this well oiled slope of coercion, control, obedience and abuse.
The import of this can not be overestimated.
References:
Position Statement on Political Abuse of Psychiatry. Paper presented at: Global Initiative on Psychiatry2005.Birley JL.
Political abuse of psychiatry. Acta psychiatrica Scandinavica. Supplementum. 2000;399:13-15.
 In Bending Science: How Special Interests Corrupt Public Health Research 1 Thomas McGarity and Wendy Wagner describe how special interest groups scheme to advance their own economic or ideological goals by using distorted or “bent” science to influence legal, regulatory and public health policy.
In Bending Science: How Special Interests Corrupt Public Health Research 1 Thomas McGarity and Wendy Wagner describe how special interest groups scheme to advance their own economic or ideological goals by using distorted or “bent” science to influence legal, regulatory and public health policy.
The authors describe a “separatist view” of science and policy that assumes scientific research is sufficiently reliable for public policy deliberations and legal proceedings when it reaches them. This is illustrated as a pipeline in which it is presumed the scientific community has properly vetted the information flow through rigorous peer-review and professional oversight. The final product that exits the pipeline is understood to be unbiased and produced in accordance with the professional norms and procedures of science. The reliability, integrity and validity of the final product is indubitably accepted. The separatist view does not consider the possibility that the scientific work exiting the pipeline could be intentionally shaped and contaminated by biasing influences as it flows through the pipeline. When this occurs the final product exiting the pipeline is distorted or “bent” and bent science can result in bad decision making and bad policy.
The separatist view does not consider the possibility that the scientific work exiting the pipeline could be intentionally shaped and contaminated by biasing influences as it flows through the pipeline. When this occurs the final product exiting the pipeline is distorted or “bent” and bent science can result in bad decision making and bad policy.
Bent science starts with a pre-determined outcome and works backward from a desired result. It is not true science. Those orchestrating the deception (“benders”) use a variety of tactics and strategies to shape, package and spin science to support their own hidden agenda and suppress opposing science.
Benders attempt to hide, dismiss and debunk contrarian research and unsupportive science. Benders will attack and harass the science and scientists that pose a threat to their interests. Using carefully crafted studies designed to confirm a desired outcome, the pre-determined conclusions are subsequently promoted and publicized to the relevant stakeholders who are often unable ( or sometimes unwilling) to discern real science from junk-science.
Misinformation, propaganda, and deception are disseminated in a variety of venues. Public relations firms are used to manipulate public perception and freelance writers are hired brandish favorable consensus statements. Authoritative reviews and critiques are ghostwritten under the names of “outside experts” who profit both monetarily and by adding a high-profile publication to their resume.
Opinion is paraded as fact and with a dearth of professional oversight the charade usually goes unnoticed and unopposed.
Data-dredging, cherry picking, confirmatory bias, confirmatory distortion, fabrication, falsification, exaggeration, and a whole host of deceptive tactics are used to work backward from an already determined result.
Any information that contradicts the answer is manipulated, undermined, suppressed or downplayed; even if it is the result of real science and evidence-based research; even if it is the truth. Professional procedure, protocol and ethics are off the table. It is an underhanded free-for-all. Bare knuckle boxing. Trash your opponents work and label it junk-science. Undermine the integrity of your opponents. Use ad hominem attacks to question the opponents motives. Claim the scientists are hacks on the take. Start rumors about them.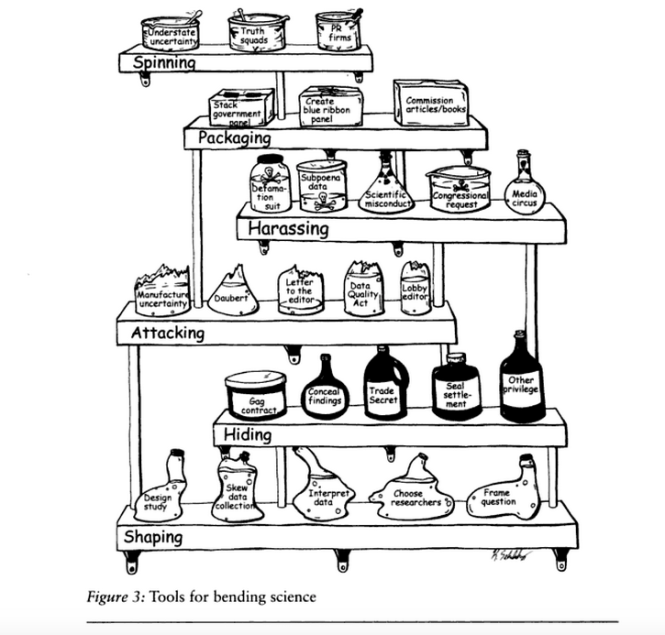 Loudly claim you are the one who is evidence based. Proclaim professionalism and authority. Quibble. Move the goalpost. Nit-pick and split hairs. Proclaim over and over and over again you are the one who is evidence based.
Loudly claim you are the one who is evidence based. Proclaim professionalism and authority. Quibble. Move the goalpost. Nit-pick and split hairs. Proclaim over and over and over again you are the one who is evidence based.
And the problem is it usually works. It is an unfair playing field. When no meaningful barriers are in place to detect cheating and identify cheaters they usually win.
Bending science can have serious and sometimes horrific consequences and multiple examples including the Tobacco and pharmaceutical industry are given in the book.
Calling for immediate action to reduce the role that bent science plays in regulatory and judicial decision making, the authors emphasize the assistance of the scientific community is necessary in designing and implementing reform.
“Shedding even a little light on how advocates bend policy -relevant science could go a long way toward remedying these problems. Indeed, precisely because the advocates have overtaken the law in this area, heightened attention to the social costs of bending science could itself precipitate significant change.”
But there are difficulties in challenging bent science including a general lack of recognition of the problem. With an absence of counter-studies to oppose deliberately manufactured ends-oriented research this would be expected.
Bent science involves the deliberate manufacturing of a pool of information designed to promote a specific agenda. A level playing field would require a pool of opposing research specifically addressing that agenda. In reality this requires both the incentive and the power to do so–an unlikely scenario short of an equally well funded competitor or sufficient public concern about the problem.
In fact counter-forces are often nonexistent. Investigatory techniques developed and promoted by the FBI crime lab (such as firearms identification and intoxication testing) is one example described in the book. These techniques evolved with little meaningful oversight from the larger scientific community and could be badly bent but there is no meaningful pool of information to disprove them. The authors aptly state that “defendants in most criminal cases lack resources to mount effective challenges, much less undertake their own counter-research.”
And part of the “art” of bending involves swaying public opinion and the mainstream media is typically aligned with the benders so opposing viewpoints seldom make the headlines.
Additionally, there is no meaningful oversight or avenue to pursue accountability. No systems exist to prevent, catch and publicly expose bent-science or those who bend science.
The influence of special interest groups on the practice of medicine is unknown. No one has examined the role of bent science in the rules, regulations, policies and decisions made by those who are in charge of the standards of medical practice and professional behavior of doctors but as a regulated profession governed by the decisions and policies of regulators it is certainly possible.
Regulation of the Medical Profession
Alexis de Toqueville once observed that a key feature of American government was the decentralized character of administration. “Written laws exist in America,” he wrote, “and one sees the daily execution of them; but although everything moves regularly, the mover can nowhere be discovered. The hand which directs the social machine is invisible.”2
Administrative law is the body of law that allows for the creation of public regulatory agencies and contains all of the statutes, judicial decisions and regulations that govern them. Administrative agencies implement their powers in the form of rules, regulations, orders and decisions. State medical boards are the regulatory agencies responsible for the licensure and discipline of physicians. They grant the right to practice medicine in the form of a medical license and each state has Medical Practice Act that governs and defines the practice of medicine. The medical board is empowered to take action against a doctor for substandard care, unprofessional behavior and other violations as defined by the state Medical Practice Act.
Administrative Code governs the licensure and disciplinary process and the State Administrative Procedure Act governs the legal process (due process, discovery, etc.). Regulatory changes are enacted through procedural, interpretive and legislative rules.
Both medical practice acts and administrative procedure acts are subject to change. Changes in medical practice acts can redefine what is acceptable practice and what constitutes professional behavior. This can increase the power and control these agencies have over doctors both professionally and socially.
Changes in Administrative practice acts can decrease what rights a doctor has if this power and control is abused. Changes in the wording of administrative code and administrative practice acts can have profound implications in these rights including due-process, timeliness of being heard, rights to appeal decisions and time-constraints for judicial review.
And when these changes occur they do so silently. The hand that directs the machine is indeed invisible. The consequences, however, are not. These changes not only impact those touched by the hand but can have a systemic impact on the entire profession.
State medical practice acts as well as administrative practice acts and code are susceptible to change and therefore susceptible to the influence of special interest groups benefitting from such change. Regulation of the medical profession is thus susceptible to bent science.
Bent Science and the Medical Profession
The impact of bent science on the regulation of the medical profession has not been studied. As a profession governed by regulatory agencies medicine is certainly not immune to the influence of special interest groups who could in turn influence public policy and regulatory decisions, rules and regulations to benefit their own interests.
Making sound decisions about regulation calls for an understanding of the problem it is intended to solve. This demands methodologically sound science and evidence-based facts arrived at through rigorous peer review and professional oversight. The science on which policy decisions are made must be reliable and unbiased. Legitimate policy must be based on recognized and legitimate institutions and experts.
If the information regulatory agencies rely on to discipline doctors and protect the public is unreliable then serious consequences can occur.
It would be beneficial to look for changes in public policy, guidelines, rules and regulations involving the medical profession and examine the reasons behind them. When did the problem present? Who presented it? Was it based on methodologically sound and accurate data? What organizations do the problem presenters represent? What organizations or individuals aligned or associated with the presenters might benefit? What are the consequences? Who is harmed?
Howard Becker describes the role of “moral entrepreneurs,” who crusade for making and enforcing rules that benefit their own interests by bringing them to the attention of the public and those in positions of power and authority under the guise of righting a society evil.8
The mechanics and mentality is similar to the science benders and, as discussed below, they use some of the same techniques.
Moral entrepreneurs take the lead in labeling a particular behavior deviant and spreading this label throughout society. They associate the behavior of some group with a society evil, affix an easily recognizable label to it and then express the conviction that the evil must be combated. Labeled as being outside the central core values of consensual society, the deviants in the designated group are perceived as posing a threat to both the values of society and society itself.
Activities can rise to the level of ‘social problems” when harm or danger is attributed to those activities and governmental powers are called upon to put an end to those harms. Bent science requires convincing others of a viewpoint and the likelihood of this occurring increases when the activity that is identified as a problem resonates with underlying societal concerns and anxieties. The problem is then endorsed by experts who give legitimacy to such claims.3,4 This legitimacy results attracts media attention which further enforces support from both the public and policy makers.5,6
As a result any bent science directed at regulatory and public policy decision making should be clearly visible.
The sociologist Stanley Cohen used the term ”moral panic” to characterize the amplification of deviance by the media, the public, and agents of social control.7 According to cultural theorist Stuart Hall, the media obtain their information from the primary definers of social reality in authoritative positions and amplify the perceived threat to the existing social order. The authorities then act to eliminate the threat.9 The dominant ideas or ideologies are reproduced by relying on the opinions of the defining authority and then spread through the media.
An internet search of what labels have been affixed to doctors in association with a threat to society there are three. A google search of “impaired physician” yields 20, 600 results; “disruptive physician” yields 17, 400 results; and “aging physician” yields 27, 800 results. A large number of these articles, opinion pieces and reviews associate impaired, disruptive and aging physicians with patient death and other adverse events, medical error, and malpractice. The labels affixed to these physicians have been characterized as a major threat to public health and the rhetorical tools used in many of these articles seems aimed at increasing public anxiety.
A PubMed search yields 154 results for the “impaired physician”; 47 results for the “disruptive physician”; and 19 results for the “aging physician.” Many of these are opinion pieces written by the same group of physicians and aimed at hospital administrators, regulators and those involved in the legal or business aspects of medicine.
There is, in fact, no evidence based research that associates the impaired, disruptive or aging physician with any adverse events. The “impaired,” “disruptive” and “aging” physician labels as evinced by a quick google search seem escalated far beyond the level warranted by the existing evidence.
The “impaired” and “disruptive” labels have taken on the status of moral panic and the “aging” label, which is being associated with cognitive impairment, seems to be heading in that direction. The number of articles being published and lectures being given on the dangers of cognitively impaired doctors is increasing. It has not yet reached the level of public awareness the impaired and disruptive have.
To acknowledge that the current level of concern about these labels is exaggerated is not to suggest they do not exist. They do. But the disparity between the evidence-base, or lack thereof, and the level of concern warrants further investigation.
To be clear, doctors who are impaired by drug and alcohol abuse need to be removed from practice to protect the public and receive treatment; doctors who are abusive to others or engage in behavior that threatens patient care need to be held accountable for their actions; and doctors who are cognitively impaired due to dementia need to be removed from practice and evaluated by the proper specialists. If a diagnosis of dementia is confirmed then they need to be removed from practice.
What is the motivation behind the “impaired,” “disruptive” and “aging” physician labels and the multiple articles linking these labels to patient harm and medical error? There is no data driven evidence so where does it come from? Could moral entrepreneurs be behind it? If so then there should be evidence of bent science and to examine this we must look for evidence that these labels have been used to influence regulatory decisions, rules, regulations and policy.
And with the recently archived Journal of Medical Regulation this task can be easily accomplished.
The Journal of Medical Regulation as Timeline and Framework for Policy Evaluation
The Federation of State Medical Boards (FSMB) is a national not-for profit organization that gives guidance to state medical boards through public policy development and recommendations on issues pertinent to medical regulation. Shortly after its founding in 1912, the Federation of State Medical Boards began publishing a quarterly journal addressing issues relating to medical licensing and regulation of doctors. First published in 1913 as the Quarterly of the Federation of State Boards of the United States, the publication has undergone several name changes and publication schedules. From1921 to 1999 it was published monthly as the Federation Bulletin. In 1999 it was changed to the quarterly Journal of Medical Licensure and Discipline and in 2010 was revised to the Journal of Medical Regulation The Journal of Medical Regulation is in the process of archiving all issues dating back to 1913.
Presently every paper dating back to 1967 is available online and the archival organization and availability of full articles published sequentially over the past half-century is historically invaluable. As the official journal of the national organization involved in the medical licensing and regulation of doctors, this archival organization allows for an unskewed and impartial examination in both historical and cultural context. We can identify when particular issues and problems were presented, who presented them and how.
The Journal of Medical Regulation archives provides a structured context to examine these issues in their historical and cultural context. This facilitates a retrospective analysis. As a timeline it allows identification of when the issues were presented. It also allows us to look at the events preceding the problem, who benefited from them, and the consequences. Could these factors be involved in influencing the regulation of medicine and shaping the medical profession? Could bent science have been involved in regulatory and administrative changes that have significantly impacted the rights and well-being of doctors and how the profession of medicine is defined? Could some of the current problems such as the marked increase in physician suicide, sham-peer review, and physician burnout be the result of bent science? If bent science is contributing to bad policy and bad decision making then it need to be exposed and addressed. Bent science is bad medicine and if it exists then we need to urgently shine a light on it.

Patterns are appearing that involve abuse of power and control of information in a system that manages all aspects of testing, assessment and treatment without oversight or regulation; an opaque and rigged game that dismisses all outside opinion with no transparency or apparent accountability (including the provision of information and justification for actions). Due process has been removed and the coercion, control and abuse of power are seen in these comments that are not only believable but plausible. This is crystal clear.
These comments can be seen here: FSPHP Response to ‘Physician Health Programs_ More Harm Than Good_’ and I urge others to read them, form their own opinions. investigate this area and help expose these issues. If PHPs are causing this degree of harm and contributing to the suicide epidemic in doctors it needs to be exposed with dispatch and allies are urgently needed.
 Source: Do physician health programs increase physician suicides? —Pamela Wible, MD
Source: Do physician health programs increase physician suicides? —Pamela Wible, MD
“Do Physician Health Programs Increase Physician Suicides?”
“Do Physician Health Programs Increase Physician Suicides?” by Dr. Pamela Wible was published on Medscape August 28, 2015 and was subsequently posted on KevinMD on September 7 where it quickly became the #1 most popular article of the week and the #3 most popular article of the past six months. 323 comments have been left on Medscape thus far and 258 on KevinMD where comments are now closed.
“Physician Health Programs: More harm Than Good?”
Pauline Anderson’s article “Physician Health Programs: More harm Than Good?” published August 19, 2015 on Medscape currently has 200 comments and the response from the President of their national organization the Federation of State Physician Health Programs (FSPHP) Doris Gunderson “FSPHP Response to ‘Physician Health Programs: More Harm than Good? published September 8 on Medscape…
View original post 1,176 more words
 Source: Do physician health programs increase physician suicides? —Pamela Wible, MD
Source: Do physician health programs increase physician suicides? —Pamela Wible, MD
“Do Physician Health Programs Increase Physician Suicides?”
“Do Physician Health Programs Increase Physician Suicides?” by Dr. Pamela Wible was published on Medscape August 28, 2015 and was subsequently posted on KevinMD on September 7 where it quickly became the #1 most popular article of the week and the #3 most popular article of the past six months. 323 comments have been left on Medscape thus far and 258 on KevinMD where comments are now closed.
“Physician Health Programs: More harm Than Good?”
Pauline Anderson’s article “Physician Health Programs: More harm Than Good?” published August 19, 2015 on Medscape currently has 200 comments and the response from the President of their national organization the Federation of State Physician Health Programs (FSPHP) Doris Gunderson “FSPHP Response to ‘Physician Health Programs: More Harm than Good? published September 8 on Medscape has generated 172 comments.
Conclusions based on comments = Increased suicide and harm by a landslide
What is the consensus so far regarding the questions raised by Anderson and Wible? Judging by the comments thus far the overwhelming consensus is that Physician Health Programs are not only causing harm but large-scale, serious, far-reaching and grave harm and this is by a landslide. Of the over 950 collective comments all but a handful have been extremely negative and critical. These comments raise specific and serious questions that are not being answered by the FSPHP or their sympathizers and apologists.
FSPHPs attempt at rebuttal with logical fallacy and authoritative opinion ineffective
Gunderson’s response to Anderson’s article deserves a point-by-point analysis at a later point, but to summarize, her rebuttal attempts to summarily dismiss the serious criticisms raised in Anderson’s article while completely avoiding the specific criticisms and dismissing key facts. She does this by questioning the integrity and quality of the both the report itself and the sources used for the report.
Calling it a “biased and unbalanced view of Physician Health Programs (PHPs)” Gunderson implies the piece falls short of the “journalistic excellence” expected of Medscape and that almost all of the information relies on “hearsay, including information from anonymous sources, allegations rather than facts, and a handful of anecdotes.” She contrasts this to the “six pages of factual information and references to several peer-reviewed articles” that were summarily ignored by Medscape.
Quality of that information aside, Anderson’s article is investigative journalism not research. It is designed to raise questions not compare outcomes. It essentially expresses the concerns of tangential dissident voices that have previously been unheard (or silenced) by the perceived authority in question and in doing so fulfills its purpose. Anderson’s paper is not a research based comparison of the literature but the exposure of criticisms involving an organization of alleged absolute power over doctors who have been stripped of due process and appeal; an organization allegedly bereft of accountability and oversight; a purported secretive unregulated system of coercion, disempowerment and control.
Most victims of this system lack the resources to even mount effective challenges, much less undertake their own counter research. Not sure what she was expecting but in situation like this allegations and anecdotes are the only ammunition available and articles such as this are the proper, and sole, means available to voice dissenting opinion and raise awareness and concern.
Gunderson predictably goes on to present the usual appeals to authority, special knowledge and consequences and inevitably brandishes the “overwhelming success” of PHPs. She also references her own study concluding that PHPs reduce malpractice. She states:
“…research demonstrates that physicians who participate in PHP monitoring for any health issue have a lower malpractice risk compared to the physician population at large, underscoring the relationship between physician health and effective patient care.”
“Overwhelming success” is of course based on Setting the Standard for Recovery: Physicians’ Health Programs, a poorly designed non-randomized non-blinded retrospective analysis of a single data set with multiple flaws in both reasoning (type I and type II errors) and statistical analysis that render its conclusions invalid. In addition the impact of undeclared but substantial financial conflicts-of-interest (including funding by drug testing and addiction treatment industries) and personal ideological biases (including personal 12-step recovery from addictions) in the authors make it nothing more than authoritative opinion. Adding the alleged misdiagnosis and over-diagnosis of addiction in physicians by this group incentivized by lucrative self-referral dollars for expensive 90-day treatment programs renders it less than authoritative opinion.
As with the “PHP-blueprint” the claims of lower malpractice risk are based on a single retrospective cohort study (with Gunderson being one of the authors ) comparing malpractice risk prior to and after being enrolled in a state PHP that revealed a reduction in malpractice rates in those who participated in the PHP. The 20% reduction they speculate:
“…could be that participants learned skills during their treatment and recovery — skills to communicate better with colleagues, staff, and patients. It may be that experience with the PHP led participants to make use of other professional supports — that is, maybe to seek consultation earlier in their work. Or maybe they were more motivated to practice conservatively and adhere to standards of practice, given what they learned in the PHP program.”
This sounds great until you consider what impact being monitored by a PHP might have on the number of patient encounters a doctor might have before and after being enrolled in a PHP. I speculate otherwise.
How many had practice restrictions, reduced hours, retired or were working in non-clinical positions after being enrolled in the PHP. Being subject to PHP monitoring is not comparable to taking a daily dose of vitamin-D. It has a very serious impact on one’s day to day activities and for a study looking at malpractice risk I would venture to guess that matching the NUMBER OF HOURS SEEING PATIENTS AND NUMBER OF PATIENT ENCOUNTERS would be an essential part of the study design that should be explicitly and accurately matched especially in a group in which the average age enrolled was 50.
This is akin to a pre-school claiming that participation in their program leads to a 20% reduction in wet diapers for children because of the skills those little fellers learned at their school.
Unfortunately this combination of logical fallacy and misrepresentation of seriously flawed studies usually sways the target. Criticisms are dismissed and everyone walks away complacent in the belief these are just good people helping doctors and protecting the public, but that is not what is happening here.
Serious questions raised and silence of FSPHP deafening.
The comments left here and on the other 3 articles have made it abundantly clear that not only is there a problem with PHPs but a very serious problem. Allegations included fabricated diagnoses, “diagnosis rigging”, “treatment rigging,” total denial of due process, lab fraud and many other serious concerns. Faced with these specific and serious criticisms and critical reasoning the FSPHP has become tongue-tied as the individual horror stories mount.
Now silence from authority is an acceptable stance when the criticisms are unreasoned and unfounded ad hominem attacks and generalizations based on bias and prejudice but that is not the case here. The testimonials and criticisms are articulate, specific and remarkably similar.
Need for further exposure, awareness and investigation through mainstream media and others
Patterns are appearing that involve abuse of power and control of information in a system that manages all aspects of testing, assessment and treatment without oversight or regulation; an opaque and rigged game that dismisses all outside opinion with no transparency or apparent accountability (including the provision of information and justification for actions). Due process has been removed and the coercion, control and abuse of power are seen in these comments that are not only believable but plausible. This is crystal clear.
These comments can be seen here: FSPHP Response to ‘Physician Health Programs_ More Harm Than Good_’ and I urge others to read them, form their own opinions. investigate this area and help expose these issues. If PHPs are causing this degree of harm and contributing to the suicide epidemic in doctors it needs to be exposed with dispatch and allies are urgently needed.
How do we care for the people who care for us? As doctors, we’re immersed in pain and suffering — as a career. We cry when our patients die. We feel grief anxiety, depression — even suicidal — all occupational hazards of our profession.
A recent Medscape article on physician health programs suggests the people who are here to help us may actually be doing more harm than good. And they may even be increasing physician suicides.
Here’s one of them:

Dear Some, My family, I love you. To others who have been good friends, I love you too. This is just the end of the line for my particular train. Earth wasn’t a great place for me. We’ll see what else is out there. Will miss you all. I’m sorry for what it’s worth. Love Greg.
On June 22, 2012. Dr. Greg Miday killed himself — 12 hours after being told not to follow his psychiatrist’s safety plan by the physician health program that controlled his medical license. Sober for years, he relapsed just before his death. A brilliant clinician, never impaired at work, Greg drank to cope with anxiety.
Afterwards, two interns jumped to their deaths from New York hospitals the same week (within three days of each other, I believe). Greg’s mother, a psychiatrist, sent this letter to the editor of the New York Times:
An unacknowledged predicament for physicians who identify their struggle with substance abuse and/or depression is that they are often placed under the supervision of their state medical board’s physician health program. My son, Greg, was being monitored by such a program. He took his own life at age 29, one week before he was to enter an esteemed oncology fellowship. His final phone calls were to the physician health program notifying them of his use of alcohol while on vacation, a disclosure he had previously described as a ‘career killer.’ These programs, which often offer no psychiatric oversight, serve as both treating and policing agencies, a serious conflict of interest. Threatened loss of licensure deters vulnerable physicians from seeking help and may even trigger a suicidal crisis. Medical Boards have the duty to safeguard the public, but the assumption that mental illness equals medical incompetence is an archaic notion. Medical Boards must stop participating in the stigmatization of mental illness. We cannot afford to lose another physician to shame.

Greg Miday and his mother, Karen Miday
The facts: Our medical schools, hospitals, and clinics actually cause or exacerbate mental health conditions in physicians, then they blame us and force us to release our confidential medical records. And in the end, they take our license ..
Maybe that’s why my friend, an excellent psychiatrist, drives 200 miles out of town, pays cash, and uses a fake name to get mental health care.
And another physician friend who was deemed “too slow” (seeing patients) by her residency director, was sent to a psychiatrist who diagnosed her with mild OCD. (Don’t we all have some OCD if we are thorough physicians?) Well, she was actually then sent to medical board who referred her to a physician health program that mandated an AA-style substance abuse program — which makes no sense at all since she does not do substances, She doesn’t drink or smoke.
So who the hell is protecting us from being misdiagnosed, mistreated, and abused?
There are many who prey upon physicians. So who cares for doctors?
And how in the world can we give patients the care we’ve never received?
Pamela Wible pioneered the community-designed ideal medical clinic and blogs at Ideal Medical Care. She is the author of Pet Goats and Pap Smears. Watch her TEDx talk, How to Get Naked with Your Doctor. She hosts the physician retreat, Live Your Dream, to help her colleagues heal from grief and reclaim their lives and careers.
“Do Physician Health Programs Increase Physician Suicides?” by Dr. Pamela Wible was published on Medscape August 28, 2015 and was subsequently posted on KevinMD on September 7, 2015 where it quickly became the #1 most popular article of the week and the #3 most popular article of the past six months. 323 comments have been left on Medscape thus far and 258 on KevinMD where comments are now closed.
Pauline Anderson’s article “Physician Health Programs: More harm Than Good?” published August 19, 2015 on Medscape currently has 200 comments and the response from the President of their national organization the Federation of State Physician Health Programs (FSPHP) Doris Gunderson “FSPHP Response to ‘Physician Health Programs: More Harm than Good? published September 8, 2015 on Medscape has generated 172 comments.
What is the consensus so far regarding the questions raised by Anderson and Wible? Judging by the comments the consensus is that Physician Health Programs are not only causing harm but serious, far-reaching and grave harm on a large scale. This is by a landslide. Of the over 950 collective comments all but a few have been extremely negative toward PHPs. They raise specific and serious questions that are not being answered by the FSPHP, their sympathizers or apologists. Gunderson’s response to Anderson’s article deserves a point-by-point analysis which will be done at a later date. To summarize, her rebuttal attempts to summarily dismiss the serious criticisms raised in Anderson’s article by questioning the integrity and quality of the both the report itself and the sources used for the report. Calling it a “biased and unbalanced view of Physician Health Programs (PHPs)” Gunderson implies the piece falls short of the “journalistic excellence” expected of Medscape and that almost all of the information relied primarily on “hearsay, including information from anonymous sources, allegations rather than facts, and a handful of anecdotes.” This is in contrast to the “six pages of factual information and references to several peer-reviewed articles” that were ignored by Medscape. Quality of that information aside, the point of Anderson’s article is to express the concerns of tangential dissident voices that often go unheard (or are silenced) by perceived authority not a research based comparison of the literature. The criticisms involve lack of due process, accountability and oversight in a secretive and unregulated system of coercion, disempowerment and control. Most victims of this system lack resources to mount effective challenges, much less undertake their own counter research. She goes on to present the usual appeals to authority, special knowledge and consequences and brandishes the “overwhelming success” of PHPs and references her own study showing that PHPs reduce malpractice stating:
“…research demonstrates that physicians who participate in PHP monitoring for any health issue have a lower malpractice risk compared to the physician population at large, underscoring the relationship between physician health and effective patient care.”
The “overwhelming success” is of course based on Setting the Standard for Recovery: Physicians’ Health Programs, a poorly designed non-randomized non-blinded retrospective analysis of a single data set with multiple flaws in both reasoning (type I and type II errors) and statistical analysis that render its conclusions invalid. In addition the impact of undeclared but substantial financial conflicts-of-interest (including funding by drug testing and addiction treatment industries) and personal ideological biases (including personal 12-step recovery from addictions) in the authors make it nothing more than authoritative opinion. Adding the alleged misdiagnosis and over-diagnosis of addiction in physicians by this group incentivized by lucrative self-referral dollars for expensive 90-day treatment programs renders it less than authoritative opinion. As with the “PHP-blueprint” the claims of lower malpractice risk are based on a single retrospective cohort study (with Gunderson being one of the authors ) that compares malpractice risk prior to and after being enrolled in the Colorado PHP and showed a reduction in malpractice in those who participated in the PHP program. The 20% reduction they speculate:
“It could be that participants learned skills during their treatment and recovery — skills to communicate better with colleagues, staff, and patients. It may be that experience with the PHP led participants to make use of other professional supports — that is, maybe to seek consultation earlier in their work. Or maybe they were more motivated to practice conservatively and adhere to standards of practice, given what they learned in the PHP program.”
This sounds great until you consider what impact being monitored by a PHP might have on the number of patient encounters a doctor might have before and after being enrolled in a PHP.
How many had practice restrictions, reduced hours, retired or were working in non-clinical positions. For a study looking at malpractice risk I would venture to guess that matching the NUMBER OF HOURS SEEING PATIENTS AND NUMBER OF PATIENT ENCOUNTERS would be an essential part of the study design. In addition the average age enrolled in the PHP was 50 and the chances of reducing hours obviously increases with time as we age.
This is like a pre-school claiming that participation in their program leads to a 20% reduction in wet diapers for children because of the skills those little fellers learned at the school.
Unfortunately this combination of logical fallacy and misrepresentation of seriously flawed studies usually sways the audience. Criticisms are dismissed with everyone complacent in the belief that these are just good people helping doctors and protecting the public. But that is not what has happened here. The comments have made it abundantly clear that not only is there a problem but a very serious problem and allegations included fabricated diagnoses, “diagnosis rigging”, “treatment rigging,” total denial of due process, lab fraud and many other serious concerns. Faced with these specific and serious criticisms and critical reason the FSPHP has become tongue-tied as the individual horror stories mount.
Now silence from authority is an acceptable stance when the criticisms are unreasoned and unfounded ad hominem attacks and generalizations based on bias and prejudice but that is not the case here. The testimonials and criticisms are articulate, specific and remarkably similar.
Patterns are appearing that involve abuse of power and control of information in a system that manages all aspects of testing, assessment and treatment without oversight or regulation; an opaque and rigged game that dismisses all outside opinion with no transparency or apparent accountability (including the provision of information and justification for actions). Due process has been removed and the coercion, control and abuse of power are seen in these comments that are not only believable but plausible. This is crystal clear.
These comments can be seen here: FSPHP Response to ‘Physician Health Programs_ More Harm Than Good_’ and I urge others to read them, form their own opinions. investigate this area and help expose these issues.
Comments (258)
RenegadeRN — I have rarely heard of a doctor even givingthat as a choice. We, as a society, are so hung up andfearful of death that we fail to see it as the natural part of …
QQQ — You want doctors to improve the quality of theirwork? Maybe if the powers that be who often partakewould BACK OFF, doctors could start reading and …
Carleton Foxx — Dr. Treadway you raise an excellent point.People learn all sorts of things from TV even when they’renot trying, so why not correct CPR form? I’m sure the …
ebrose — Either the authors have drunk the Kool-Aid orthey have been hitting the samples closet in the office. As aretired physician (internist/pulmonologist) who …