
From Bullyonline.org read this
Symptoms of Post Traumatic Stress Disorder (PTSD)
Complex Post Traumatic Stress Disorder, PTSD symptoms, survivor guilt and trauma caused by bullying, harassment, abuse and abusive life experiences
What is Post Traumatic Stress Disorder?
How do I recognise the symptoms of PTSD? How do I recover from PTSD?
Updated 4 November 2005
Please link to this page: stress/ptsd.htm
On this page
Definition of Post Traumatic Stress Disorder – what is PTSD?
DSM-IV diagnostic criteria for Post Traumatic Stress Disorder
Causes of Post Traumatic Stress Disorder
Complex PTSD, PDSD and bullying
Mapping the health effects of bullying onto the diagnostic criteria for PTSD
Common symptoms of Post Traumatic Stress Disorder (PTSD)
Associated symptoms of PTSD – survivor guilt etc
New!Transformation
The difference between mental breakdown and stress breakdown
Differences between mental illness and psychiatric injury
Features of Complex PTSD specific to bullying, especially feelings of guilt
Post Traumatic Stress Disorder and fatigue
Incidence of PTSD and Complex PTSD in the general population
Legal aspects of Post Traumatic Stress Disorder
Bullying causes PTSD: the legal case
Complex PTSD and stress, especially stress at work
David Kinchin’s book Post Traumatic Stress Disorder: the invisible injury
Tim Field’s book Bully in sight validates the experience of psychological violence
Recommended reading on PTSD | Bookshops | Articles on PTSD
Seminars on Post Traumatic Stress Disorder and recovery
Links to PTSD, Complex PTSD and trauma sites
“When the trauma is inflicted by another person, is especially intense, or the traumatized person is extremely close to the trauma, the severity of traumatization may be especially profound”
Robert C Scaer, MD, Author, The Body bears the Burden: Trauma, Dissociation and Disease
Definition
Post Traumatic Stress Disorder (PTSD) is a natural emotional reaction to a deeply shocking and disturbing experience. It is a normal reaction to an abnormal situation.
Post Traumatic Stress Disorder (PTSD) is defined in DSM-IV, the fourth edition of the American Psychiatric Association’s Diagnostic and Statistical Manual. For a doctor or mental health professional to be able to make a diagnosis, the condition must be defined in DSM-IV or its international equivalent, the World Health Organization’s ICD-10.
In the previous version of DSM (DSM-III) a criterion of Post Traumatic Stress Disorder was for the sufferer to have faced a single major life-threatening event; this criterion was present because a) it was thought that PTSD could not be a result of “normal” events such as bereavement, business failure, interpersonal conflict, bullying, harassment, stalking, marital disharmony, working for the emergency services, etc, and b) most of the research on PTSD had been undertaken with people who had suffered a threat to life (eg combat veterans, especially from Vietnam, victims of accident, disaster, and acts of violence).
In DSM-IV the requirement was eased although most mental health practitioners continue to interpret diagnostic criterion A1 as applying only to a single major life-threatening event. There is growing recognition that Post Traumatic Stress Disorder can result from many types of emotionally shocking experience including an accumulation of small, individually non-life-threatening events in which case the resultant PTSD is referred to as Complex PTSD.
DSM-IV diagnostic criteria for Post Traumatic Stress Disorder (PTSD)
The diagnostic criteria for Post Traumatic Stress Disorder (PTSD) are defined in DSM-IV as follows:
A. The person experiences a traumatic event in which both of the following were present:
1. the person experienced or witnessed or was confronted with an event or events that involved actual or threatened death or serious injury, or a threat to the physical integrity of self or others;
2. the person’s response involved intense fear, helplessness, or horror.
B. The traumatic event is persistently re-experienced in any of the following ways:
1. recurrent and intrusive distressing recollections of the event, including images, thoughts or perceptions;
2. recurrent distressing dreams of the event;
3. acting or feeling as if the traumatic event were recurring (eg reliving the experience, illusions, hallucinations, and dissociative flashback episodes, including those on wakening or when intoxicated);
4. intense psychological distress at exposure to internal or external cues that symbolise or resemble an aspect of the traumatic event;
5. physiological reactivity on exposure to internal or external cues that symbolise or resemble an aspect of the traumatic event.
C. Persistent avoidance of stimuli associated with the trauma and numbing of general responsiveness (not present before the trauma) as indicated by at least three of:
1. efforts to avoid thoughts, feelings or conversations associated with the trauma;
2. efforts to avoid activities, places or people that arouse recollections of this trauma;
3. inability to recall an important aspect of the trauma;
4. markedly diminished interest or participation in significant activities;
5. feeling of detachment or estrangement from others;
6. restricted range of affect (eg unable to have loving feelings);
7. sense of a foreshortened future (eg does not expect to have a career, marriage, children or a normal life span).
D. Persistent symptoms of increased arousal (not present before the trauma) as indicated by at least two of the following:
1. difficulty falling or staying asleep;
2. irritability or outbursts of anger;
3. difficulty concentrating;
4. hypervigilance;
5. exaggerated startle response.
E. The symptoms on Criteria B, C and D last for more than one month.
F. The disturbance causes clinically significant distress or impairment in social, occupational or other important areas of functioning.
The focus of the DSM-IV definition of Post Traumatic Stress Disorder is a single life-threatening event or threat to integrity. However, the symptoms of traumatic stress also arise from an accumulation of small incidents rather than one major incident. Examples include:
- repeated exposure to horrific scenes at accidents or fires, such as those endured by members of the emergency services (eg bodies mutilated in car crashes, or horribly burnt or disfigured by fire, or dismembered or disembowelled in aeroplane disasters, etc)
- repeated involvement in dealing with serious crime, eg where violence has been used and especially where children are hurt
- breaking news of bereavement caused by accident or violence, especially if children are involved
- repeated violations such as in verbal abuse, physical abuse, emotional abuse and sexual abuse
- regular intrusion and violation, both physical and psychological, as in bullying, stalking, harassment, domestic violence, etc
Where the symptoms are the result of a series of events, the term Complex PTSD (formerly referred to unofficially as Prolonged Duress Stress Disorder or PDSD) may be more appropriate. Whilst Complex PTSD is not yet an official diagnosis in DSM-IV or ICD-10, it is often used in preference to other terms such as “rolling PTSD”, “PDSD”, and “cumulative stress”. See the National Center for PTSD fact page on Complex PTSD.
Causes of PTSD
PTSD resulting from accident, disaster, war, terrorism, torture, kidnap, etc has been extensively studied and literature is available elsewhere. The first written reference to PTSD symptoms comes from the sixth century BC; Post Traumatic Stress Disorder is nothing new – and neither is the willingness of some people to discredit and deny the existence of the disorder.
This section of Bully OnLine focuses on PTSD and Complex PTSD resulting from bullying, primarily in the workplace, however anyone suffering PTSD (however caused) will find this page enlightening.
Most of the information on this page and web site is relevant to other types of bullying, eg at school, in relationships (including domestic violence), by families, by neighbours or landlords, in the care of the elderly, in the armed services, etc. Bullying is behind harassment, discrimination, prejudice and persecution, therefore targets of repeated sexual harassment or racial discrimination or religious or ethnic persecution will also identify with the symptoms. The insight about bullying on this web site is therefore also relevant to more serious issues including physical abuse, repeated verbal abuse, sexual abuse, violent crime, kidnap, abduction, rape, war, terrorism, torture, and denial and abuse of human rights. Those exploring Contact Experience may also find this page helpful.
PTSD, Complex PTSD and bullying
It’s widely accepted that PTSD can result from a single, major, life-threatening event, as defined in DSM-IV. Now there is growing awareness that PTSD can also result from an accumulation of many small, individually non-life-threatening incidents. To differentiate the cause, the term “Complex PTSD” is used. The reason that Complex PTSD is not in DSM-IV is that the definition of PTSD in DSM-IV was derived using only people who had suffered a single major life-threatening incident such as Vietnam veterans and survivors of disasters.
Note: there has recently been a trend amongst some psychiatric professionals to label people suffering Complex PTSD as a exhibiting a personality disorder, especially Borderline Personality Disorder. This is not the case – PTSD, Complex or otherwise, is apsychiatric injury and nothing to do with personality disorders. If there is an overlap, thenBorderline Personality Disorder should be regarded as a psychiatric injury, not a personality disorder. If you encounter a psychiatrist, psychologist or other mental health professional who wants to label your Complex PTSD as a personality disorder, change to another, more competent professional.
It seems that Complex PTSD can potentially arise from any prolonged period of negative stress in which certain factors are present, which may include any of captivity, lack of means of escape, entrapment, repeated violation of boundaries, betrayal, rejection, bewilderment, confusion, and – crucially – lack of control, loss of control and disempowerment. It is the overwhelming nature of the events and the inability (helplessness, lack of knowledge, lack of support etc) of the person trying to deal with those events that leads to the development of Complex PTSD. Situations which might give rise to Complex PTSD include bullying, harassment, abuse, domestic violence, stalking, long-term caring for a disabled relative, unresolved grief, exam stress over a period of years, mounting debt, contact experience, etc. Those working in regular traumatic situations, eg the emergency services, are also prone to developing Complex PTSD.
A key feature of Complex PTSD is the aspect of captivity. The individual experiencing trauma by degree is unable to escape the situation. Despite some people’s assertions to the contrary, situations of domestic abuse and workplace abuse can be extremely difficult to get out of. In the latter case there are several reasons, including financial vulnerability (especially if you’re a single parent or main breadwinner – the rate of marital breakdown is approaching 50% in the UK), unavailability of jobs, ageism (many people who are bullied are over 40), partner unable to move, and kids settled in school and you are unable or unwilling to move them. The real killer, though, is being unable to get a job reference – the bully will go to great lengths to blacken the person’s name, often for years, and it is this lack of reference more than anything else which prevents people escaping.
Until recently, little (or no) attention was paid to the psychological harm caused by bullying and harassment. Misperceptions (usually as a result of the observer’s lack of knowledge or lack of empathy) still abound: “It’s something you have to put up with” (like rape or repeated sexual abuse?) and “Bullying toughens you up” (ditto). Armed forces personnel faced threats of being labelled with “cowardice” and “lack of moral fibre” (LMF) if they gave in to the symptoms of PTSD. In World War I, 306 British and Commonwealth soldiers were shot as “cowards” and “deserters” on the orders of General Haig in an act which today would be treated as a war crime – seeseparate page on this injustice.
In the UK at least 16 children kill themselves each year because they are being bullied at school. This figure is established in the book Bullycide: death at playtime. Each of these deaths is unnecessary, foreseeable, and preventable. The UK has one of the highest adult suicide rates in Europe: around 5000 a year. The number of adults in the UK committing suicide because of bullying is unknown. Each year 19,000 children attempt suicide in the UK – one every half hour. in the UK, suicide is the number one cause of death for 18-24-year-old males. Females also attempt suicide in large numbers but tend to use less successful means.
Since Andrea Adams first identified workplace bullying and gave it its name in 1988, recognition of adult bullying has grown steadily. Tim Field’s UK National Workplace Bullying Advice Line has logged over 8000 cases in seven years; in the majority of cases (over 80%), the caller is a white-collar worker who has become the prey of a serial bully whosebehaviour profile suggests a disordered personality. Callers refer to predecessors who have had stress breakdowns, taken early or ill-health retirement, or been dismissed on grounds of ill-health – all caused by the same individual. Sometimes callers refer to suicides of fellow employees.
Mapping the health effects of bullying onto PTSD and Complex PTSD
Repeated bullying, often over a period of years, results in symptoms of Complex Post Traumatic Stress Disorder. How do the PTSD symptoms resulting from bullying meet the criteria in DSM-IV?
A. The prolonged (chronic) negative stress resulting from bullying has lead to threat of loss of job, career, health, livelihood, often also resulting in threat to marriage and family life. The family are the unseen victims of bullying.
A.1.One of the key symptoms of prolonged negative stress is reactive depression; this causes the balance of the mind to be disturbed, leading first to thoughts of, then attempts at, and ultimately, suicide.
A.2.The target of bullying may be unaware that they are being bullied, and even when they do realise (there’s usually a moment of enlightenment as the person realises that the criticisms and tactics of control etc are invalid), they often cannot bring themselves to believe they are dealing with a disordered personality who lacks a conscience and does not share the same moral values as themselves. Naivety is the great enemy. The target of bullying is bewildered, confused, frightened, angry – and after enlightenment, very angry. For an answer to the question Why me? click here.
B.1. The target of bullying experiences regular intrusive violent visualisations and replays of events and conversations; often, the endings of these replays are altered in favour of the target.
B.2. Sleeplessness, nightmares and replays are a common feature of being bullied.
B.3. The events are constantly relived; night-time and sleep do not bring relief as it becomes impossible to switch the brain off. Such sleep as is achieved is non-restorative and people wake up as tired, and often more tired, than when they went to bed.
B.4. Fear, horror, chronic anxiety, and panic attacks are triggered by any reminder of the experience, eg receiving threatening letters from the bully, the employer, or personnel about disciplinary hearings etc.
B.5. Panic attacks, palpitations, sweating, trembling, ditto.
Criteria B4 and B5 manifest themselves as immediate physical and mental paralysis in response to any reminder of the bullying or prospect of having to take action against the bully.
C. Physical numbness (toes, fingertips, lips) is common, as is emotional numbness (especially inability to feel joy). Sufferers report that their spark has gone out and, even years later, find they just cannot get motivated about anything.
C.1. The target of bullying tries harder and harder to avoid saying or doing anything which reminds them of the horror of the bullying.
C.2. Work, especially in the person’s chosen field becomes difficult, often impossible, to undertake; the place of work holds such horrific memories that it becomes impossible to set foot on the premises; many targets of bullying avoid the street where the workplace is located.
C.3. Almost all callers to the UK National Workplace Bullying Advice Line report impaired memory; this may be partly due to suppressing horrific memories, and partly due to damage to the hippocampus, an area of the brain linked to learning and memory (see John O’Brien’s paper below)
C.4. the person becomes obsessed with resolving the bullying experience which takes over their life, eclipsing and excluding almost every other interest.
C.5. Feelings of withdrawal and isolation are common; the person just wants to be on their own and solitude is sought.
C.6. Emotional numbness, including inability to feel joy (anhedonia) and deadening of loving feelings towards others are commonly reported. One fears never being able to feel love again.
C.7. The target of bullying becomes very gloomy and senses a foreshortened career – usually with justification. Many targets of bullying ultimately give up their career; in the professions, severe psychiatric injury, severely impaired health, refusal by the bully and the employer to give a satisfactory reference, and many other reasons, conspire to bar the person from continuance in their chosen career.
D.1. Sleep becomes almost impossible, despite the constant fatigue; such sleep as is obtained tends to be unsatisfying, unrefreshing and non-restorative. On waking, the person often feels more tired than when they went to bed. Depressive feelings are worst early in the morning. Feelings of vulnerability may be heightened overnight.
D.2. The person has an extremely short fuse and is often permanently irritated, especially by small insignificant events. The person frequently visualises a violent solution, eg arranging an accident for, or murdering the bully; the resultant feelings of guilt tend to hinder progress in recovery.
D.3. Concentration is impaired to the point of precluding preparation for legal action, study, work, or search for work.
D.4. The person is on constant alert because their fight or flight mechanism has become permanently activated.
D.5. The person has become hypersensitized and now unwittingly and inappropriately perceives almost any remark as critical.
E. Recovery from a bullying experience is measured in years. Some people never fully recover.
F. For many, social life ceases and work becomes impossible; the overwhelming need to earn a living combined with the inability to work deepens the trauma.
Common symptoms of PTSD and Complex PTSD that sufferers report experiencing
- hypervigilance (may feel like paranoia, but see HERE for key differences between paranoia and hypervigilance)
- exaggerated startle response
- irritability
- sudden angry or violent outbursts
- flashbacks, nightmares, intrusive recollections, replays, violent visualisations
- triggers
- sleep disturbance
- exhaustion and chronic fatigue
- reactive depression
- guilt
- feelings of detachment
- avoidance behaviours
- nervousness, anxiety
- phobias about specific daily routines, events or objects
- irrational or impulsive behaviour
- loss of interest
- loss of ambition
- anhedonia (inability to feel joy and pleasure)
- poor concentration
- impaired memory
- joint pains, muscle pains
- emotional numbness
- physical numbness
- low self-esteem
- an overwhelming sense of injustice and a strong desire to do something about it
Associated symptoms of Complex PTSD
Survivor guilt: survivors of disasters often experience abnormally high levels of guilt for having survived, especially when others – including family, friends or fellow passengers – have died. Survivor guilt manifests itself in a feeling of “I should have died too”. In bullying, levels of guilt are also abnormally raised. The survivor of workplace bullying may have develop an intense albeit unrealistic desire to work with their employer (or, by now, their former employer) to eliminate bullying from their workplace. Many survivors of bullying cannot gain further employment and are thus forced into self-employment; excessive guilt may then preclude the individual from negotiating fair rates of remuneration, or asking for money for services rendered. The person may also find themselves being abnormally and inappropriately generous and giving in business and other situations.
Shame, embarrassment, guilt, and fear are encouraged by the bully, for this is how all abusers – including child sex abusers – control and silence their victims.
Marital disharmony: the target of bullying becomes obsessed with understanding and resolving what is happening and the experience takes over their life; partners become confused, irritated, bewildered, frightened and angry; separation and divorce are common outcomes.
Breakdown
The word “breakdown” is often used to describe the mental collapse of someone who has been under intolerable strain. There is usually an (inappropriate) inference of “mental illness”. All these are lay terms and mean different things to different people. I define two types of breakdown:
Nervous breakdown or mental breakdown is a consequence of mental illness
Stress breakdown is a psychiatric injury, which is a normal reaction to an abnormal situation
The two types of breakdown are distinct and should not be confused. A stress breakdown is a natural and normal conclusion to a period of prolonged negative stress; the body is saying “I’m not designed to operate under these conditions of prolonged negative stress so I am going to do something dramatic to ensure that you reduce or eliminate the stress otherwise your body may suffer irreparable damage; you must take action now”. A stress breakdown is often predictable days – sometimes weeks – in advance as the person’s fear, fragility, obsessiveness, hypervigilance and hypersensitivity combine to evolve into paranoia (as evidenced by increasingly bizarre talk of conspiracy or MI6). If this happens, a stress breakdown is only days or even hours away and the person needs urgent medical help. The risk of suicide at this point is heightened.
Often the cause of negative stress in an organisation can be traced to the behaviour of one individual. The profile of this individual is on the serial bully page. I believe bullying is the main – but least recognised – cause of negative stress in the workplace today. To see the effects of prolonged negative stress on the body click here.
The person who suffers a stress breakdown is often treated as if they have had a mental breakdown; they are sent to a psychiatrist, prescribed drugs used to treat mental illness, and may be encouraged – sometimes coerced or sectioned – into becoming a patient in a psychiatric hospital. The sudden transition from professional working environment to a ward containing schizophrenics, drug addicts and other people with genuine long-term mental health problems adds to rather than alleviates the trauma. Words like “psychiatrist”, “psychiatric unit” etc are often translated by work colleagues, friends, and sometimes family into “nutcase”, “shrink”, “funny farm”, “loony” and other inappropriate epithets. The bully encourages this, often ensuring that the employee’s personnel record contains a reference to the person’s “mental health problems”. Sometimes, the bully produces their own amateur diagnosis of mental illness – but this is more likely to be a projection of the bully’s own state of mind and should be regarded as such.
During the First World War, British soldiers suffering PTSD and stress breakdown were labelled as “cowards” and “deserters”. During the Second World War, soldiers suffering PTSD and stress breakdowns were again vilified with these labels; Royal Air Force personnel were labelled as “lacking moral fibre” and their papers stamped “LMF”. For further commentary on this issue, click here. It’s noticeable that those administrators and top brass enforcing this labelling were themselves always situated a safe distance from the fighting; see the section on projection.
The person who is being bullied often thinks they are going mad, and may be encouraged in this belief by those who do not have that person’s best interests at heart. They are not going mad; PTSD is an injury, not an illness.
Sometimes, the term “psychosis” is applied to mental illness, and the term “neurosis” to psychiatric injury. The main difference is that a psychotic person is unaware they have a mental problem, whereas the neurotic person is aware – often acutely. The serial bully’s lack of insight into their behaviour and its effect on others has the hallmarks of a psychosis, although this obliviousness would appear to be a choice rather than a condition. With targets of bullying, I prefer to avoid the words “neurosis” and “neurotic”, which for non-medical people have derogatory connotations. Hypersensitivity and hypervigilance are likely to cause the person suffering PTSD to react unfavourably to the use of these words, possibly perceiving that they, the target, are being blamed for their circumstances.
A frequent diagnosis of stress breakdown is “brief reactive psychosis”, especially if paranoia and suicidal thoughts predominate. However, a key difference between mental breakdown and stress breakdown is that a person undergoing a stress breakdown will be intermittently lucid, often alternating seamlessly between paranoia and seeking information about their paranoia and other symptoms. The person is also likely to be talking about resolving their work situation (which is the cause of their problems), planning legal action against the bully and the employer, wanting to talk to their union rep and solicitor, etc.
Transformation
A stress breakdown is a transformational experience which, with the right support, can ultimately enrich the experiencer’s life. However, completing the transformation can be a long and sometimes painful process. The Western response – to hospitalise and medicalize the experience, thus hindering the process – may be well-intentioned, but may lessen the value and effectiveness of the transformation. How would you feel if, rather than a breakdown, you viewed it as a breakthrough? How would you feel if it was suggested to you that the reason for a stress breakdown is to awaken you to your mission in life and to enable you to discover the reason why you have incarnated on this planet? How would it change your view of things if it was also suggested to you that a stress breakdown reconfigures your brain to enable you to embark on the path that will culminate in the achievement of your mission? [More | More]
Differences between mental illness and psychiatric injury
The person who is being bullied will eventually say something like “I think I’m being paranoid…“; however they are correctly identifying hypervigilance, a symptom of PTSD, but using the popular but misunderstood word paranoia. The differences between hypervigilance and paranoia make a good starting point for identifying the differences between mental illness and psychiatric injury.
Our new page on Organised Gang Stalking and Mind Control explains the difference between “gang stalking”, a conspiracy theory, and bullying and other forms of abuse. The differences are analogous to the differences between paranoia and hypervigilance.
|
Paranoia
|
Hypervigilance
|
- paranoia is a form of mental illness; the cause is thought to be internal, eg a minor variation in the balance of brain chemistry
|
- is a response to an external event (violence, accident, disaster, violation, intrusion, bullying, etc) and therefore an injury
|
- paranoia tends to endure and to not get better of its own accord
|
- wears off (gets better), albeit slowly, when the person is out of and away from the situation which was the cause
|
- the paranoiac will not admit to feeling paranoid, as they cannot see their paranoia.
|
- the hypervigilant person is acutely aware of their hypervigilance, and will easily articulate their fear, albeit using the incorrect but popularised word “paranoia”
|
- sometimes responds to drug treatment
|
- drugs are not viewed favourably by hypervigilant people, except in extreme circumstances, and then only briefly; often drugs have no effect, or can make things worse, sometimes interfering with the body’s own healing process
|
- the paranoiac often has delusions of grandeur; the delusional aspects of paranoia feature in other forms of mental illness, such as schizophrenia
|
- the hypervigilant person often has a diminished sense of self-worth, sometimes dramatically so
|
- the paranoiac is convinced of their self-importance
|
- the hypervigilant person is often convinced of their worthlessness and will often deny their value to others
|
- paranoia is often seen in conjunction with other symptoms of mental illness, butnot in conjunction with symptoms of PTSD
|
- hypervigilance is seen in conjunction with other symptoms of PTSD, but not in conjunction with symptoms of mental illness
|
- the paranoiac is convinced of their plausibility
|
- the hypervigilant person is aware of how implausible their experience sounds and often doesn’t want to believe it themselves (disbelief and denial)
|
- the paranoiac feels persecuted by a person or persons unknown (eg “they’re out to get me”)
|
- the hypervigilant person is hypersensitized but is often aware of the inappropriateness of their heightened sensitivity, and can identify the person responsible for their psychiatric injury
|
|
|
- heightened sense of vulnerability to victimisation
|
- the sense of persecution felt by the paranoiac is a delusion, for usually no-one is out to get them
|
- the hypervigilant person’s sense of threat is well-founded, for the serial bully is out to get rid of them and has often coerced others into assisting, eg through mobbing; the hypervigilant person often cannot (and refuses to) see that the serial bully is doing everything possible to get rid of them
|
- the paranoiac is on constant alert because they know someone is out to get them
|
- the hypervigilant person is on alert in case there is danger
|
- the paranoiac is certain of their belief and their behaviour and expects others to share that certainty
|
- the hypervigilant person cannot bring themselves to believe that the bully cannot and will not see the effect their behaviour is having; they cling naively to the mistaken belief that the bully will recognise their wrongdoing and apologise
|
Other differences between mental illness and psychiatric injury include:
|
Mental illness
|
Psychiatric injury
|
- the cause often cannot be identified
|
- the cause is easily identifiable and verifiable, but denied by those who are accountable
|
- the person may be incoherent or what they say doesn’t make sense
|
- the person is often articulate but prevented from articulation by being traumatised
|
- the person may appear to be obsessed
|
- the person is obsessive, especially in relation to identifying the cause of their injury and both dealing with the cause and effecting their recovery
|
- the person is oblivious to their behaviour and the effect it has on others
|
- the person is in a state of acute self-awareness and aware of their state, but often unable to explain it
|
- the depression is a clinical or endogenous depression
|
- the depression is reactive; the chemistry is different to endogenous depression
|
- there may be a history of depression in the family
|
- there is very often no history of depression in the individual or their family
|
- the person has usually exhibited mental health problems before
|
- often there is no history of mental health problems
|
- may respond inappropriately to the needs and concerns of others
|
- responds empathically to the needs and concerns of others, despite their own injury
|
- displays a certitude about themselves, their circumstances and their actions
|
- is often highly sceptical about their condition and circumstances and is in a state of disbelief and bewilderment which they will easily and often articulate (“I can’t believe this is happening to me” and “Why me?” – click here for the answer)
|
- may suffer a persecution complex
|
- may experience an unusually heightened sense of vulnerability to possible victimisation (ie hypervigilance)
|
- suicidal thoughts are the result of despair, dejection and hopelessness
|
- suicidal thoughts are often a logical and carefully thought-out solution or conclusion
|
|
|
- is driven by the anger of injustice
|
- often doesn’t look forward to each new day
|
- looks forward to each new day as an opportunity to fight for justice
|
- is often ready to give in or admit defeat
|
- refuses to be beaten, refuses to give up
|
Common features of Complex PTSD from bullying
People suffering Complex PTSD as a result of bullying report consistent symptoms which further help to characterise psychiatric injury and differentiate it from mental illness. These include:
Fatigue with symptoms of or similar to Chronic Fatigue Syndrome (formerly ME)
An anger of injustice stimulated to an excessive degree (sometimes but improperly attracting the words “manic” instead of motivated, “obsessive” instead of focused, and “angry” instead of “passionate”, especially from those with something to fear)
An overwhelming desire for acknowledgement, understanding, recognition and validation of their experience
A simultaneous and paradoxical unwillingness to talk about the bullying (clickhere to see why) or abuse (click here to see why)
A lack of desire for revenge, but a strong motivation for justice
A tendency to oscillate between conciliation (forgiveness) and anger (revenge) with objectivity being the main casualty
Extreme fragility, where formerly the person was of a strong, stable character
Numbness, both physical (toes, fingertips, and lips) and emotional (inability to feel love and joy)
Clumsiness
Forgetfulness
Hyperawareness and an acute sense of time passing, seasons changing, and distances travelled
An enhanced environmental awareness, often on a planetary scale
An appreciation of the need to adopt a healthier diet, possibly reducing or eliminating meat – especially red meat
Willingness to try complementary medicine and alternative, holistic therapies, etc
A constant feeling that one has to justify everything one says and does
A constant need to prove oneself, even when surrounded by good, positive people
An unusually strong sense of vulnerability, victimisation or possible victimisation, often wrongly diagnosed as “persecution”
Occasional violent intrusive visualisations
Feelings of worthlessness, rejection, a sense of being unwanted, unlikeable and unlovable
A feeling of being small, insignificant, and invisible
An overwhelming sense of betrayal, and a consequent inability and unwillingness to trust anyone, even those close to you
In contrast to the chronic fatigue, depression etc, occasional false dawns with sudden bursts of energy accompanied by a feeling of “I’m better!”, only to be followed by a full resurgence of symptoms a day or two later
Excessive guilt – when the cause of PTSD is bullying, the guilt expresses itself in forms distinct from “survivor guilt”; it comes out as:
- an initial reluctance to take action against the bully and report him/her knowing that he/she could lose his/her job
- later, this reluctance gives way to a strong urge to take action against the bully so that others, especially successors, don’t have to suffer a similar fate
- reluctance to feel happiness and joy because one’s sense of other people’s suffering throughout the world is heightened
- a proneness to identifying with other people’s suffering
- a heightened sense of unworthiness, undeservingness and non-entitlement (some might call this shame)
- a heightened sense of indebtedness, beholdenness and undue obligation
- a reluctance to earn or accept money because one’s sense of poverty and injustice throughout the world is heightened
- an unwillingness to take ill-health retirement because the person doesn’t want to believe they are sufficiently unwell to merit it
- an unwillingness to draw sickness, incapacity or unemployment benefit to which the person is entitled
- an unusually strong desire to educate the employer and help the employer introduce an anti-bullying ethos, usually proportional to the employer’s lack of interest in anti-bullying measures
- a desire to help others, often overwhelming and bordering on obsession, and to be available for others at any time regardless of the cost to oneself
- an unusually high inclination to feel sorry for other people who are under stress, including those in a position of authority, even those who are not fulfilling the duties and obligations of their position (which may include the bully) but who are continuing to enjoy salary for remaining in post [hint: to overcome this tendency, every time you start to feel sorry for someone, say to yourself “sometimes, when you jump in and rescue someone, you deny them the opportunity to learn and grow”]
Fatigue
The fatigue is understandable when you realise that in bullying, the target’s fight or flight mechanism eventually becomes activated from Sunday evening (at the thought of facing the bully at work on Monday morning) through to the following Saturday morning (phew – weekend at last!). The fight or flight mechanism is designed to be operational only briefly and intermittently; in the heightened state of alert, the body consumes abnormally high levels of energy. If this state becomes semi-permanent, the body’s physical, mental and emotional batteries are drained dry. Whilst the weekend theoretically is a time for the batteries to recharge, this doesn’t happen, because:
- the person is by now obsessed with the situation (or rather, resolving the situation), cannot switch off, may be unable to sleep, and probably has nightmares, flashbacks and replays;
- sleep is non-restorative and unrefreshing – one goes to sleep tired and wakes up tired
- this type of experience plays havoc with the immune system; when the fight or flight system is eventually switched off, the immune system is impaired such that the person is open to viruses which they would under normal circumstances fight off; the person then spends each weekend with a cold, cough, flu, glandular fever, laryngitis, ear infection etc so the body’s batteries never have an opportunity to recharge.
When activated, the body’s fight or flight response results in the digestive, immune and reproductive systems being placed on standby. It’s no coincidence that people experiencing constant abuse, harassment and bullying report malfunctions related to these systems (loss of appetite, constant infections, flatulence, irritable bowel syndrome, loss of libido, impotence, etc). The body becomes awash with cortisol which in high prolonged doses is toxic to brain cells. Cortisol kills off neuroreceptors in the hippocampus, an area of the brain linked with learning and memory. The hippocampus is also the control centre for the fight or flight response, thus the ability to control the fight or flight mechanism itself becomes impaired.
Most survivors of bullying experience symptoms of Chronic Fatigue Syndrome – seehealth page for details.
Legal
In law, gaining compensation for psychiatric injury is a long arduous process which can take five years of more. The areas most commonly quoted are breach of duty of care under the Health and Safety at Work Act (1974), and personal injury. There is little case law for personal injury caused by bullying (although there have been settlements which are subject to gagging clauses).
The most frequently quoted case is Walker v. Northumberland County Council [1995] IRLR35 (High Court). John Walker was a social worker dealing with child abuse cases. He suffered a stress breakdown caused by work overload, recovered and went back to work; his employer, having been informed of the cause of his stress breakdown, took no steps to reduce his workload and Mr Walker subsequently suffered a second stress breakdown. The award was made by the courts on the basis of the second stress breakdown.
In May 2001 the case of Long v. Mercury Mobile Communications Services resulted in Mr Long (the target of bullying, in this case in the form of a vendetta) winning his case on the basis of a first stress breakdown. This has become the new precedent. The House of Lords judgment in Barber v. Somerset County Council has also set a new precedent.
In July 1999 Beverley Lancaster won her case for stress against Birmingham City Council, and in September 2000 in the case of Waters v. London Metropolitan Police the UK House of Lords judged that an employee (or in this case an office holder) has the right in law to sue for negligence if bullying and harassment which the employer knew about but failed to deal with resulted in psychiatric injury.
However, the law at present is clearly inadequate:
the better a person qualifies to pursue a claim for personal injury by satisfying PTSD DSM-IV diagnostic criteria B4, B5, C1, C2, C3, D3, E and F, the more they are, ipso facto, frustrated from pursuing the claim
B4. intense psychological distress at exposure to internal or external cues that symbolise or resemble an aspect of the traumatic event;
B5. physiological reactivity on exposure to internal or external cues that symbolise or resemble an aspect of the traumatic event.
C. Persistent avoidance of stimuli associated with the trauma and numbing of general responsiveness:
C1. efforts to avoid thoughts, feelings or conversations associated with the trauma;
C2. efforts to avoid activities, places or people that arouse recollections of this trauma;
C3. inability to recall an important aspect of the trauma;
D3. difficulty concentrating;
E. The symptoms on Criteria B, C and D last for more than one month.
F. The disturbance causes clinically significant distress or impairment in social, occupational or other important areas of functioning.
The Diagnostic Criteria are exacerbated by the abusive and aggressive behaviour of the bully, the employer, and the employer’s legal representatives in their defence and rejection of the claim.
In its Consultation Paper on Liability for Psychiatric Illness (No 137) the Law Commission recommended, among other things, that
6.2 There should continue to be liability for negligently inflicted psychiatric illness that does not arise from a physical injury to the plaintiff;
6.15 Damages for psychiatric illness should continue to be recoverable irrespective of whether the psychiatric illness is of a particular severity;
6.20 Subject to standard defences, there should be liability where an employer has negligently overburdened its employee with work thereby foreseeably causing him or her to suffer a psychiatric illness.
There are a growing number of personal injury cases (for psychiatric injury caused by bullying) in the pipeline, with the first settled out of court in February 1998. See the case law page for recent cases and settlements.
New! Bullying causes PTSD: the legal case
Many people, especially guilty parties and their accomplices and lawyers, reject the notion that PTSD can arise from bullying. However, this research proves otherwise:
- European Journal of Work and Organizational Psychology (EJWOP), 1996, 5(2), whole issue devoted to bullying and its effects, including PTSD. Published by Psychology Press, 27 Church Road, Hove, East Sussex BN3 2FA, UK.
- The late Professor Heinz Leymann was one of the first people to identify the symptoms of injury to health caused by bullying as PTSD.
- Research from Warwick University, England, identifies bullying as a cause of PTSD
- Bullied workers suffer ‘battle stress’ and show the same symptoms of armed forces personnel who have been engaged in war
It is common practice for employers to order targets of bullying to see a psychiatrist of the employers’ choosing and to have the employee diagnosed as being “mentally ill” in order to provide grounds for dismissal whilst thwarting a personal injury claim. See BMA: ethics advice and the articles Abuse of Medical Assessments to Dismiss Whistleblowers andBattered Plaintiffs – injuries from hired guns and compliant courts and Giving Workers the Treatment: if you raise a stink, you go to a shrink!
Incidence of PTSD and Complex PTSD
The number of people suffering PTSD is unknown but David Kinchin estimates in his book Post Traumatic Stress Disorder: the invisible injury that at any time around 1% of the population are experiencing PTSD. This figure is only for PTSD resulting from traditional causes such as accident, violence or disaster.
The incidence of Complex PTSD is unknown; with estimates of the number of people being bullied at work in the UK ranging from 1 in 8 (IPD, November 1996) to 1 in 2 (Staffordshire University Business School, 1994), the figure could be as high as 14 million – or more. The silent suffering is considerable; symptoms prevent sufferers from realising their potential and contributing fully to society. Many sufferers are claiming benefit, often reluctantly, as people who suffer Complex PTSD are often hard working and industrious prior to their injury. Anyone who is on benefit and unable to work is also not paying tax and national insurance.
Within some groups of society, the incidence of PTSD must be expected to be much higher than one per cent. Within the emergency services (fire, police and ambulance) and the armed forces (army, navy and air force) the incidence of PTSD can be as high as 15 per cent. It is a disturbing probability that out of every hundred police officers currently engaged in uniformed patrol duties in our towns and cities, fifteen will be suffering from symptoms in accord with PTSD.
David Kinchin, Author, Post Traumatic Stress Disorder
Stress
Stress is on everybody’s minds these days. However, whilst almost everyone seems to feel “stressed”, most people are unaware that stress comes in two forms: positive and negative.
Positive stress (what Abraham Maslow calls eustress) is the result of good management and excellent leadership where everyone works hard, is kept informed and involved, and – importantly – is valued and supported. People feel in control.
Negative stress (what Maslow calls distress) is the result of a bullying climate where threat and coercion substitute for non-existent management skills. When people use the word “stress” on its own, they usually mean “negative stress”.
I define stress as “the degree to which one feels, perceives or believes one is not in control of one’s circumstances”. Control – or people’s perception of being in control – seems to be key to susceptibility to experiencing PTSD.
The UK, and much of the Western world, adopts a blame-the-victim mentality as a way of avoiding having to deal with difficult issues. When dealing with stress it is essential to identify the cause of stress and work to reduce or eliminate the cause. Sending employees on stress management courses may sound good on paper but coercing people to endure more stress without addressing the cause is going to result in further psychiatric injury.
Stress is not the employee’s inability to cope with excessive workload and excessive demands but a consequence of the employer’s failure to provide a safe system of work as required by the Health and Safety at Work Act 1974.
Stress is known to cause brain damage. Dr John T O’Brien, consultant in old-age psychiatry at Newcastle General Hospital, published a paper in March 1997 entitled “The glucocorticoid cascade hypothesis in man” (and presumably woman), helpfully subtitled “Prolonged stress may cause permanent brain damage”.
If Dr O’Brien’s research proves correct, then employers who encourage stressful regimes comprising long hours, threat and coercion might soon find themselves on the wrong end of a string of expensive personal injury lawsuits.
Further discussion of stress is on the health page.
Understanding and recovering from Post Traumatic Stress Disorder (PTSD)

Post Traumatic Stress Disorder
The invisible injury, 2005 edition
by
David Kinchin
ISBN 0952912147
Published by Success Unlimited 2004
Paperback, 16 chapters, 224 pages, resources, index
Click book cover (left) for more information
“This is the book I so badly wanted when I was traumatised.”
David Kinchin, Author
Few people realise that trauma and psychiatric injury can be more devastating and long-lasting than physical injury. Traumatic events strike unexpectedly turning everyday experiences upside-down and destroying the belief that ‘it could never happen to me’.
PTSD is a natural emotional reaction to a deeply shocking and disturbing experience after which it can be difficult to believe that life will ever be the same again. The symptoms are surprisingly common and include sleep problems, nightmares and waking early, flashbacks and replays, impaired memory, inability to concentrate, hypervigilance (feels like but isnot paranoia), jumpiness and an exaggerated startle response, fragility and hypersensitivity, detachment and avoidance behaviours, depression, irritability, violent outbursts, joint and muscle pains, panic attacks, fatigue, low self-esteem, feelings of nervousness and undue anxiety. Survivors endure abnormal feelings of guilt, perhaps for having survived when those around them didn’t.
Untreated, PTSD symptoms can last a lifetime, impairing health, damaging relationships and preventing people achieving their potential. Sufferers often find that knowledge and treatment of PTSD (and especially Complex PTSD) is difficult to obtain. However, prospects for recovery are good when you have the right counsel and are in the company of fellow survivors and those with genuine insight, empathy and experience.
Now in its fourth edition, Post Traumatic Stress Disorder: the invisible injury furnishes PTSD sufferers (and their carers, families and professionals) with knowledge, belief and advice to hasten recovery, re-establish relationships and enable people to once more find meaning, purpose and pleasure in life.
Post Traumatic Stress Disorder: the invisible injury is a reassuring and sensitively-written book which validates, explains and relieves the silent unseen psychological suffering of trauma and is essential reading for survivors of accident, disaster, violence, rape, bullying, physical abuse, sexual abuse, crime, abduction, kidnap, terrorism, war, torture, bereavement, trauma, and those witnessing such events. Their rescuers, relatives, families, carers, counsellors and therapists will also gain insight into the suffering endured by their loved ones or clients.
This book provides a unique insight for anyone working in the areas of healthcare, social work, employment, personnel and HR, legal services, research and victim support as well as those in the emergency services, uniformed services, rescue services, critical incident debriefing and traumatic incident reduction.
Anyone suffering unusual levels of stress and anxiety will also find relief in this clear and enlightening text, as will those with an interest in stress, psychiatric injury, and the Disability Discrimination Act.
David Kinchin’s Post Traumatic Stress Disorder: the invisible injury, 2004 edition is a revised and updated edition of Post Traumatic Stress Disorder: a practical guide to recoverypublished by Thorsons in 1994 and the republished edition Post Traumatic Stress Disorder: the invisible injury, published by Success Unlimited in 1998 and 2001.
Order a copy:
Online with secure credit card ordering
By fax or letter with printed order form
How bullying and harassment at school cause psychiatric injury, trauma, PTSD, and suicide
 Bullycide
Bullycide
Death at playtime
An exposé of child suicide caused by bullying
by
Neil Marr and Tim Field
Introduction by Jo Brand
ISBN 0952912120
Published by Success Unlimited in January 2001
Paperback, 18 chapters, 320 pages, 30 b/w pictures, resources, index
Click book cover (left) for more details
“An excellent book.”
Times Education Supplement, May 2001
“Require reading in every LEA [Local Education Authority] in the UK.”
Yorkshire Evening Post, March 2001
Using a blend of powerful testimony, moving narrative, insightful analysis and practical advice, Bullycide: death at playtime reveals the full and long-lasting extent of the psychiatric injury caused by bullying at school and in childhood. Contains new interviews with bereaved families, survivors and people who have overcome the trauma of bullying at school to succeed in life – sometimes spectacularly. Includes initiatives to combat bullying, helplines, organisations, suggested reading and web sites.
More reviews and reader feedback
Order a copy:
Online with secure credit card ordering
By fax or letter with printed order form
Identifying and dealing with workplace bullying, harassment and injury to health

Bully in sight
How to predict, resist, challenge and combat workplace bullying
Overcoming the silence and denial by which abuse thrives
by Tim Field
Foreword by Diana Lamplugh OBE
ISBN 0952912104
Published by Success Unlimited 1996, reprinted 1998, 1999 and 2001
Paperback, 16 chapters, 384 pages, resources, index
Click book cover (left) for more details
“Thank you for writing Bully in sight … it’s like a torch in the darkness.”
“I have been through a horrendous 6 years, and for the last 2 years your website and book have been my lifeline. Your insight into the bully’s behaviour is incredible. You deserve all the praise you get and more! I am still battling but I know now that I am right and the bullies are wrong.”
More readers’ feedback and comments.
Bully in sight identifies bullying as the common denominator of harassment, discrimination, prejudice, abuse, conflict and violence, and describes the principal perpetrator of psychological violence, the serial bully.Bully in sight is one of the first books to describe psychiatric injury and Post Traumatic Stress Disorder resulting from long-term bullying.
Written with the experience and insight only a fellow experiencer can impart, Bully in sight validates the experience of bullying when everyone else is trying to ignore or deny it.
Packed with insight, ideas, guidance and direction, plus sources of help and suggested reading.
Order a signed copy:
Online with secure credit card ordering
By fax or letter with printed order form
Further reading on psychiatric injury
Post Traumatic Stress Disorder: the invisible injury, 2005 edition, David Kinchin, Success Unlimited, 2004, ISBN 0952912147
Supporting Children with Post-traumatic Stress Disorder: a practical guide for teachers and professionals, David Kinchin and Erica Brown, David Fulton Publishers, £12.00, ISBN 1853467278
Stress and employer liability, Earnshaw & Cooper, IPD, 1996, £16.95, ISBN 0852926154 (updated edition in preparation)
Why zebras don’t get ulcers: an updated guide to stress, stress-related diseases, and coping, Robert M Sapolsky, Freeman, 1998, ISBN 0716732106
The Body Bears the Burden: Trauma, Dissociation and Disease, Robert C Scaer, MD, The Haworth Medical Press, NY, ISBN 0789012464
Recovering damages for psychiatric injury, M Napier & K Wheat, Blackstone Press, £19.95, ISBN 1854313525
Understanding stress breakdown, Dr William Wilkie, Millennium Books, 1995
Understanding stress, V Sutherland & C Cooper, Chapman and Hall
Trauma and transformation: growing in the aftermath of suffering, R Tedeschi & L Calhoun, Sage, 1996
The Railway Man, Eric Lomax, Vintage, 1996, ISBN 0099582317 (a poignant story of undiagnosed PTSD from World War II)
Bookshops and services
The Oxford Stress and Trauma Centre bookshop
The Inner Bookshop, 111 Magdalen Road, Oxford OX4 1RQ: mind, body, spirit, esoteric, holistic, paranormal, contact experience etc.
Articles
European Journal of Work and Organizational Psychology (EJWOP), 1996, 5(2), whole issue devoted to bullying and its effects, including PTSD. Published by Psychology Press, 27 Church Road, Hove, East Sussex BN3 2FA, UK.
British Journal of Psychiatry, (1997), 170, 199-201, The ‘glucocorticoid cascade’ hypothesis in man: prolonged stress may cause permanent brain damage, Dr John T O’Brien MRCPsych, Department of Psychiatry and Institute for the Health of the Elderly, University of Newcastle.
Cortisol – keeping a dangerous hormone in check, David Tuttle, LE Magazine July 2004
T cells divide and rule in Gulf War syndrome (and asthma, TB, cancer, ME), Jenny Bryan, Immunology section in The Biologist, (1997) 44 (5)
Traumatic stress under-recognised
5% of males and 10% of females will develop PTSD in their lifetime says the National Institute for Clinical Excellence (NICE): http://news.bbc.co.uk/1/hi/health/4373367.stm
Seminars and workshops
David Kinchin’s own web page and PTSD workshops
Links
The late Professor Heinz Leymann was one of the world’s pioneers and foremost authorities on mobbing (bullying) and PTSD, with over a decade of experience. His web site is essential reading for anyone studying the effects of bullying on health.
David Kinchin, author of Post traumatic Stress Disorder: the invisible injury, 2004 edition
BBC News Online: bullying at school causes PTSD, name calling and verbal abuse worse than physical bullying
Ex-soldier Michael New wins £620,000 damages for PTSD: http://news.bbc.co.uk/1/hi/wales/4725455.stm
US soldiers return from Iraq with PTSD: http://news.bbc.co.uk/1/hi/world/americas/4474715.stm
Untreated PTSD may mean a lifetime of impoverished physical health including heart disease and cancer: http://news.bbc.co.uk/1/hi/health/4179602.stm
Bullied workers suffer ‘battle stress’ and show the same symptoms of armed forces personnel who have been engaged in war: http://news.bbc.co.uk/1/hi/business/3563450.stm
National Center for PTSD factsheets:
Complex PTSD – recommended.
Coping with PTSD and Recommended Lifestyle Changes for PTSD Patients: http://www.ncptsd.org/facts/treatment/fs_coping.html
Anger and trauma: http://www.ncptsd.org/facts/specific/fs_anger.html
You can join the NCPTSD mailing list to be alerted to updates on PTSD information at their site.
Post Traumatic Stress Disorder diagnostic criteria and self-diagnosis at Internet Mental Health.
Helpguide for Post-traumatic Stress Disorder (PTSD): Symptoms, Types and Treatment
High percentage of youth in the USA report symptoms of Post Traumatic Stress and other disorders; study involving 4,023 adolescents finds that exposure to interpersonal violence (including bullying) increases the risk for PTSD.
PTSD Public Service Announcement Website
Patience Press aims to ensure that other people never have to be alone with the pain of PTSD, struggling to heal without help or support.
The Traumatic Stress Clinic in London has good online information about PTSD.
UK Trauma Group web site.
Contact information about local specialist resources in the UK offering advice about the assessment or treatment of people with psychological reactions to major traumatic events.
NICE guidelines for PTSD: http://www.nice.org.uk/page.aspx?o=248505
Traumatic Incident Reduction – the web site of Gerald D French.
Hospital Anxiety and Depression Scale (HADS): a simple, standardised self-assessment questionnaire for measuring the severity of anxiety and depression.
CODT – Cooperative Online Dictionary of Trauma, a dictionary of trauma terms:
The National Institute for Clinical Excellence (NICE) page on Post Traumatic Stress Disorder (PTSD).
For some time the American Psychological Association (APA) has been looking at the traumatic effects of psychological violence
American Psychiatric Association (APA) public information on Posttraumatic Stress Disorder
Dave Baldwin’s site at http://www.trauma-pages.com/ contains comprehensive links.
A Valuable Stress Information Resource Website
Stress Spot is a stress information resource with links to Post Traumatic Stress Disorder web sites.
The Panic Center.
Brain Injury Resource Center page on Post Traumatic Stress Disorder
The Trauma Center in Alston, Massachusetts. The Medical Director of the Trauma Center is Dr Bessel van der Kolk.
Trauma in the Family by Family Trauma Group Centre.
Partners with PTSD by Frank Ochberg, M.D.
The trauma of betrayal
Why a broken heart hurts so much; social rejection may affect your brain as much as physical pain
Legal Abuse Syndrome: how the courts and legal system may cause Post Traumatic Stress Disorder
Essentials for litigating Post Traumatic Stress Disorder (PTSD) claims: http://www.lawandpsychiatry.com/html/Litigating%20PTSD%20Claims%20-%20Final.pdf
Pre-action protocol for disease/illness claims: http://www.apil.com/pdf/publicdocs/DISEASE_PROTOCOL_approved_version.pdf
Descriptions of Post Traumatic Stress Disorder (PTSD) and Acute Stress Disorder (ASD).
Gift From Within is a private, non-profit organization dedicated to those who suffer post-traumatic stress disorder (PTSD), those at risk for PTSD, and those who care for traumatized individuals.
TACT is the UK Trauma After Care Trust.
Regular verbal abuse more damaging than physical assault: research from Warwick University, England.
Articles from Psychology Today: When Disaster Strikes by Hara Estroff Marano, Recovering From Trauma andLife Lessons by Ellen McGrath Ph.D., plus Trauma Do’s and Don’ts
“A Guide to Anxiety Disorders” – http://www.datehookup.com/content-a-guide-to-anxiety-disorders.htm has a concise compilation of information on a variety of common anxiety disorders
Trauma is covered on the Mental Health Network at http://www.mhnet.org/guide/trauma.htm
The Healing Centre Online is at http://www.healing-arts.org/
Ask the Internet Therapist
Institute of Psychiatry library listing on traumatic stress.
The International Society for Traumatic Stress Studies (ISTSS) has a comprehensive web site on various aspects of trauma and its causes.
The European Society for Traumatic Stress Studies (ESTSS) web site.
The Invisible Epidemic: Post-Traumatic Stress Disorder, Memory and the Brain by J. Douglas Bremner, M.D.
Information for for ex-servicemen & servicewomen who think they are suffering from PTSD.
A glossary of trauma terms
PTSD and dissociation
Information on Falsification of Type (Dr Carl Gustav Jung’s description for an individual whose most developed and/or used skills were outside one’s area of greatest natural preference) and PASS (Prolonged Adaption Stress Syndrome) is at http://www.benziger.org/pass.html
Rebecca Coffey’s PTSD bibliography at http://www.sover.net/~schwcof/ptsd.html
Canadian Traumatic Stress Network page at http://play.psych.mun.ca/~dhart/trauma_net/index.html and the useful web connections page athttp://play.psych.mun.ca/~dhart/trauma_net/useful.html
Australian Trauma Web is at http://www.psy.uq.edu.au/PTSD
Links to PTSD and PTSD-related sites are at http://www.ptsd.com/
Gillian Kelly, barrister at law, looks at the development of Post Traumatic Stress Disorder and the legal recognition thereof on her web site athttp://www.telecoms.net/law/index.html
Hope E. Morrow’s Trauma Central contains a large collection of links to online articles on trauma and related subjects.
Risk Factors in PTSD and Related Disorders: Theoretical, Treatment, and Research Implications, Anne M Dietrich MA, Doctoral Candidate, University of British Columbia, Canada
See the ability, not the disability list of PTSD links
If your health has suffered but those around you cannot or will not see your hurt, see Why Seeing Is Not Believing When Dealing With A Chronic Illness
PTSD may be a flaw in the way the brain is designed: http://www.mhsanctuary.com/ptsd/ineng.htm
The Highly Sensitive Person (HSP): http://www.artdsm.com/hsp/
Copyright © Tim Field 1996-2005. Information on this site may be reproduced freely for non-commercial purposes – please acknowledge the source by quoting the web site address ptsd.htm
The views on this web site are those of Tim Field and result from personal experience of being bullied out of his job and experiencing a stress breakdown caused by the bullying, thereafter setting up and running theUK National Workplace Bullying Advice Line since January 1996 and Bully OnLine since 1997, and liaising with over 10,000 cases of bullying. I believe this to be the largest number of targets of workplace bullying that any one person has ever dealt with. I am not a mental health professional. Whilst every effort has been made to ensure accuracy, no responsibility can be accepted. In all matters, consult a qualified competent professional.
Please link to this page and help us increase its visibility in the search engines:
ptsd.htm
Stress, injury to health, trauma and PTSD
How bullying, harassment and abuse damage health and cause trauma
Stress, trauma and PTSD Home Page
The cause of stress revealed
Stress at work, injury to health, fatigue, depression, suicide
PTSD (Post Traumatic Stress Disorder) and Complex PTSD
Bullying, stress and self-harm |Stress and debility
Bullying and suicide | Cases of suicide caused by bullying
Bullying shame | Bullying fear | Bullying embarrassment |Bullying guilt
Bullying and denial |Trauma | Shell shock: PTSD in WW1
David Kinchin’s book Post Traumatic Stress Disorder: the invisible injury
validates and relieves the silent unseen suffering of trauma
Profile of David Kinchin |PTSD workshops by David Kinchin
Neil Marr and Tim Field’s book Bullycide: death at playtime reveals the
secret toll of children who attempt or commit suicide because of bullying
Home Pages
The Field Foundation | Bully OnLine
Workplace bullying |School bullying |Family bullying
Bullying news | Press and media centre
Bullying case histories |Bullying resources
Stress, PTSD and psychiatric injury
Action to tackle bullying |Related issues
Success Unlimited
Books on bullying and related issues
Trauma and spiritual growth
















 In addition to an up to date medication list we decided to put in the bare but essential elements of the medical record that would be needed in an emergency; these consisted of demographics, emergency contacts, a basic problem list, allergies and a baseline EKG.
In addition to an up to date medication list we decided to put in the bare but essential elements of the medical record that would be needed in an emergency; these consisted of demographics, emergency contacts, a basic problem list, allergies and a baseline EKG. They don’t see the problem and they don’t see a need for a solution. Many believe it is the patient’s responsibility to keep track of their medications and that any problem associated with not providing their medication list up to date were self-inflicted.” He said it will be a different story in five or ten years when the problem is acknowledged and accepted by the rank and file.
They don’t see the problem and they don’t see a need for a solution. Many believe it is the patient’s responsibility to keep track of their medications and that any problem associated with not providing their medication list up to date were self-inflicted.” He said it will be a different story in five or ten years when the problem is acknowledged and accepted by the rank and file.















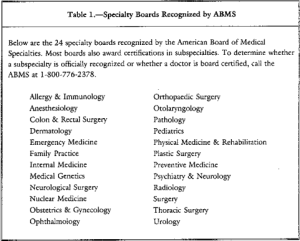

 The field of psychology also defines strict guidelines for board certification. The American Board of Professional Psychology was incorporated in 1947 with the support of the American Psychological Association. The ABPP is a unitary governing body of separately incorporated specialty examining boards which assures the establishment, implementation, and maintenance of specialty standards and examinations by its member boards. Through its Central Office, a wide range of administrative support services are provided to ABPP Boards, Board-certified specialists, and the public. Specialization in a defined area within the practice of psychology connotes competency acquired through an organized sequence of formal education, training, and experience. In order to qualify as a specialty affiliated with the ABPP, a specialty must be represented by an examining board which is stable, national in scope, and reflects the current development of the specialty. A specialty board is accepted for affiliation following an intensive self-study and a favorable review by the ABPP affirming that the standards for affiliation have been met. These standards include a thorough description of the area of practice and the pattern of competencies required therein as well as requirements for education, training, and experience, the research basis of the specialty, practice guidelines, and a demonstrated capacity to examine candidates for the specialty on a national level.
The field of psychology also defines strict guidelines for board certification. The American Board of Professional Psychology was incorporated in 1947 with the support of the American Psychological Association. The ABPP is a unitary governing body of separately incorporated specialty examining boards which assures the establishment, implementation, and maintenance of specialty standards and examinations by its member boards. Through its Central Office, a wide range of administrative support services are provided to ABPP Boards, Board-certified specialists, and the public. Specialization in a defined area within the practice of psychology connotes competency acquired through an organized sequence of formal education, training, and experience. In order to qualify as a specialty affiliated with the ABPP, a specialty must be represented by an examining board which is stable, national in scope, and reflects the current development of the specialty. A specialty board is accepted for affiliation following an intensive self-study and a favorable review by the ABPP affirming that the standards for affiliation have been met. These standards include a thorough description of the area of practice and the pattern of competencies required therein as well as requirements for education, training, and experience, the research basis of the specialty, practice guidelines, and a demonstrated capacity to examine candidates for the specialty on a national level.