She likes a rigged game, you know what I mean?”
— R.P. Murphy in Ken Kesey’s One Flew Over the Cuckoo’s Nest
 An article published in the March 17, 2014 newsletter Alcoholism and Drug Abuse Weekly entitled “Physician group urges focus on spiritual and psychosocial” describes a group of doctors emphasizing “that for all addictions, the psychosocial and spiritual interventions, including 12-step interventions must be included in the treatment process.” “According to founding board member Dr. Ken Thompson, M.D., “to not do so falls short of practicing good addiction medicine.”
An article published in the March 17, 2014 newsletter Alcoholism and Drug Abuse Weekly entitled “Physician group urges focus on spiritual and psychosocial” describes a group of doctors emphasizing “that for all addictions, the psychosocial and spiritual interventions, including 12-step interventions must be included in the treatment process.” “According to founding board member Dr. Ken Thompson, M.D., “to not do so falls short of practicing good addiction medicine.”
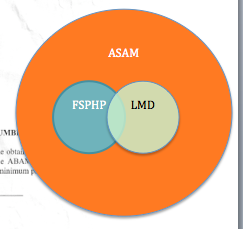
With a “significant percentage” in 12-step recovery themselves, “they have formed group called “Like-Minded Docs.” This group now has close to 300 physicians, “many of whom are medical directors of top treatment programs and also members of the American Society of Addiction Medicine (ASAM).”
ADAW March 17 2014

Dr. Thompson is the Medical Director of Caron treatment center in Pennsylvania. The group also includes medical directors of many other treatment centers including Hazelden, Talbott, Marworth, and Promises. The President of the American Society of Addiction Medicine is in fact a Like-Minded Doc.
The number of like-minded docs represent over 10% of the American Society of Addiction Medicine (ASAM).
Ostensibly I applaud the ideal of addressing the psychosocial and spiritual aspects of addiction.
I also acknowledge that alcoholics anonymous and 12-step recovery is a treatment tool that can provide great benefit to some people. But to others it provides no benefit and to some it can cause harm. As most reasonable people would agree, forcing individuals into a thought process of spirituality should never be mandated.
That being said, I have no strong feelings for or against A.A and 12-step spirituality. I view it through the same pluralistic and open-minded lens as I do religion–there are many paths to salvation and none superior.
I have referred patients to A.A. and see it as an option and a personal choice that can provide great benefit to some people, none to others and in fact harm those who are not aligned with the concept.
If it works for you great. If not then let’s take a different approach.
Although the ideals of the Like-Minded Docs are laudable, it is the framework that is concerning as it creates a confluence of currents that preclude option and choice.
It is a scaffold that can be used for coercion, control, and imposition. It can be abused.
And this is exactly what is being done in many of the State Physician Health Programs (PHPs) as well as the drug courts. It is notable that many of the same individuals pushing PHPs as a “replicable” model of recovery are the very same individuals behind the drug courts and the motivation behind this does not appear to be altruism but power and greed.
Originally funded by state medical societies and staffed by volunteer physicians, PHP’s were designed to help sick doctors and protect the public. Over the past decade these programs have undergone a sweeping transformation due to this subgroup of the ASAM.
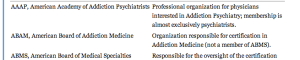
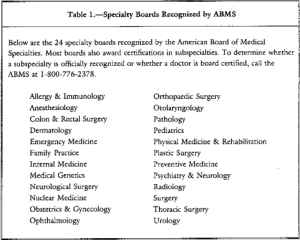
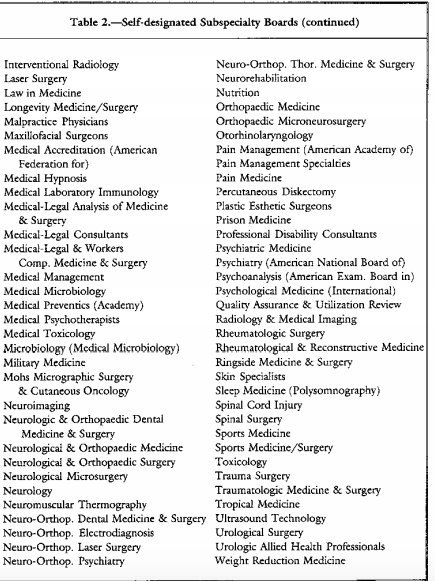
It is important to understand that the ASAM is not recognized by the American Board of Medical Specialties (ABMS). They created their own “board certification” (ABAM) and the only requirement is an M.D. in any specialty and some sort of experience in substance abuse. This is not a medical specialty but a “special interest group.”
 Trumpeting the false dichotomy that addiction is a “brain disease” and not a “moral failing” while portraying themselves as altruistic advocates of the afflicted, this subgroup of the ASAM has cultivated an organization that exudes authority, knowledge, respectability, and advocacy. But they are an illegitimate authority and others must be made cognizant of this fact.
Trumpeting the false dichotomy that addiction is a “brain disease” and not a “moral failing” while portraying themselves as altruistic advocates of the afflicted, this subgroup of the ASAM has cultivated an organization that exudes authority, knowledge, respectability, and advocacy. But they are an illegitimate authority and others must be made cognizant of this fact.
The ASAM has set forth definitions of addiction, shaped diagnostic criteria, dictated assessment protocols and shaped public policy all under the guise of scholarship and compassion. But is this the real motive? I don’t think so.
This same group introduced junk science such as the EtG and PEth alcohol biomarkers through Greg Skipper, FSPHP, ASAM, and a like-Minded Doc who can also be found on this list. The conflicts-of-interest are serious and vast.

This same group has created the “impaired” physician construct as well as the “moral panic” of a hidden cadre of drug addled and besotted doctors protected by a “culture of silence” that has seriously damaged the reputation of doctors and the medical profession through the eyes of both regulators and the general public.
This same group has introduced and promulgated the nebulous “disruptive physician” and successfully fostered a moral crusade to attack this huge apparently hidden but non-existent threat.
The next target is the “aging physician” and if you do an internet search you will see they are currently fomenting a call to arms to root out senility in medicine.
This same group used the same tactics in each case.
With no evidence base they used propaganda and disinformation to convince regulatory and administrative medicine that witches are real, witches are dangerous, and that they were the experts when it came to identifying, assessing and treating witches. And it worked.
By infiltrating state PHPs they have become the might and main of addiction medicine in the United States.
By removing dissenters who disagreed with the groupthink they have taken over almost all of the state PHPs organized under the Federation of State Physician Health Programs (FSPHP).
And this is where it becomes interesting.
 State PHPs are very strict when it comes to choice in rehabilitation facilities for for physicians in need of assessment and treatment for substance abuse.
State PHPs are very strict when it comes to choice in rehabilitation facilities for for physicians in need of assessment and treatment for substance abuse.
In fact there is no choice in the matter.
As home to some of the countries top ranked hospitals and most prestigious medical schools Massachusetts is an international healthcare hub with world-class teaching, research, and clinical care.
Two of the top three psychiatric hospitals in the United States as rated by U.S. News and World Report are found here in Massachusetts with McLean Hospital earning the top prize and Massachusetts General Hospital ranked number three.
However, this medical mecca of learning and research is apparently unable to attract anyone with competence and skill to assess physicians for substance abuse or disruptive behavior.
In Massachusetts if the State PHP, PHS,inc. feels a physician is in need of an assessment the evaluation must be done at “a facility experienced in the assessment and treatment of health care professionals” It must be done at a “PHP-approved” facility. No exceptions.
And apparently these esoteric skills are only found in Georgia, Arkansas, Alabama, and a half dozen other places.
With over 20 years experience with the Massachusetts PHP, Physicians Health Services, inc., Harvard Medical Schools Dr.’s John Knight and J. Wesley Boyd wrote an article in the Journal of Addiction Medicine last year concerning ethical issues in state PHPs.
Ethical and Managerial Considerations Regarding State Physician Health Programs
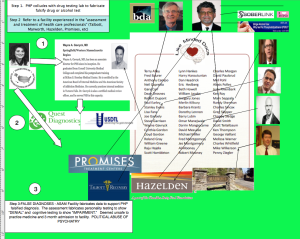 One of the issues Knight and Boyd discussed was the conflicts of interest between the state PHPs and the evaluation centers.
One of the issues Knight and Boyd discussed was the conflicts of interest between the state PHPs and the evaluation centers.
One comment I was surprised got past editorial review was that the treatment centers may “consciously or otherwise” tailor diagnosis and recommendations to the PHP’s impression of that physician. “Consciously” tailoring a diagnosis is fraud. It is political abuse of psychiatry.
If you look up the medical directors of the “preferred facilities” and then cross reference with the list of LMD’s you get a perfect match.
So when the PHP refers a physician for an evaluation and gives them a choice of an assessment facility there is no choice.
It is three card monte. It is a shell game. Heads I win tails you lose.
The ASAM has imposed the prohibitionist chronic brain disease spiritual recovery model of addiction on the field of medicine.
It is a system of coercion, control, and indoctrination. And another ASAM Like-Minded Doc, Robert Dupont, is calling this the “new paradigm” of addiction medicine and wants to spread it out to other venues including schools.
Like-Minded Docs solves the final piece of the puzzle. It explains why so many doctors across the country are claiming fabrication and manipulation of personality and cognitive tests to support nonexistent diagnoses.
They are not gathering data to form a hypothesis but making data fit a hypothesis that arrived before they did.
It also explains the marked increase in physician suicide.
With guilt assumed from the start, no due process, no appeal and no way out physicians are being bullied, demoralized, and dehumanized by these zealots to the point of hopelessness.
This needs to stop.
Medicine is predicated on competence, good-faith, and integrity. Medical ethics necessitates beneficence, respect, and autonomy. The scaffold erected here is designed for coercion and control. Exposure, transparency, and accountability are urgent. An evidence based Cochrane type assessment of their “research” and an Institute of Medicine Conflict of Interest review are long overdue.
The emperor has no clothes and sunshine is the best disinfectant.



 This dicto simpliciter argument can, in fact, be refuted simply by pointing it out! Sadly, no one ever did so the ASAM front-group hasbeen able to establish this caricature of the arrogant paternalistic know it all needing 3 months or more of treatment as standard of care for our profession. They did this by getting medical boards and the FSMB to accept fantasy as fact by relying on board members tendency to accept expert evidence at face value–which they always do and that is a personality characteristic that I would argue is not dicto simpliciter.
This dicto simpliciter argument can, in fact, be refuted simply by pointing it out! Sadly, no one ever did so the ASAM front-group hasbeen able to establish this caricature of the arrogant paternalistic know it all needing 3 months or more of treatment as standard of care for our profession. They did this by getting medical boards and the FSMB to accept fantasy as fact by relying on board members tendency to accept expert evidence at face value–which they always do and that is a personality characteristic that I would argue is not dicto simpliciter.







 Trumpeting the false dichotomy that addiction is a “brain disease” and not a “moral failing” while portraying themselves as altruistic advocates of the afflicted, this subgroup of the ASAM has cultivated an organization that exudes authority, knowledge, respectability, and advocacy. But they are an illegitimate authority and others must be made cognizant of this fact.
Trumpeting the false dichotomy that addiction is a “brain disease” and not a “moral failing” while portraying themselves as altruistic advocates of the afflicted, this subgroup of the ASAM has cultivated an organization that exudes authority, knowledge, respectability, and advocacy. But they are an illegitimate authority and others must be made cognizant of this fact.
 State PHPs are very strict when it comes to choice in rehabilitation facilities for for physicians in need of assessment and treatment for substance abuse.
State PHPs are very strict when it comes to choice in rehabilitation facilities for for physicians in need of assessment and treatment for substance abuse.
 One of the issues Knight and Boyd discussed was the conflicts of interest between the state PHPs and the evaluation centers.
One of the issues Knight and Boyd discussed was the conflicts of interest between the state PHPs and the evaluation centers.


 The Plan to… Require Doctors to Drug-Test all Patients
The Plan to… Require Doctors to Drug-Test all Patients

 To evaluate the legitimacy of an authority it is necessary to:
To evaluate the legitimacy of an authority it is necessary to:


 The concept of denial is not just used to force people into treatment and justify abuse during treatment but to suppress specific questions and deliberately avoid key facts.
The concept of denial is not just used to force people into treatment and justify abuse during treatment but to suppress specific questions and deliberately avoid key facts.